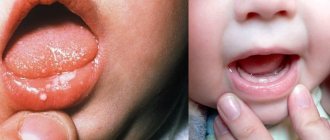
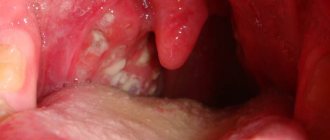
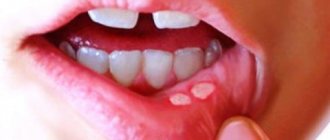
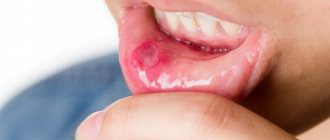
To understand what allergic stomatitis , it is necessary to clarify two concepts.
Allergy. An excessive protective reaction of the body's immune system to certain external substances foreign to the body, called allergens. These may be substances that are essentially harmless to humans, but for some people (allergy sufferers) they are perceived by the immune system as dangerous to the body. In immunology, there are several types of allergic reactions, but in practical allergology only type I (fast or instant reaction) and type IV (slow or delayed reaction) are relevant. These types of reactions in the body can occur separately, but they can also occur in parallel. In addition, symptoms similar to those of allergies can be caused by other pathologies, for example, pseudoallergic diseases, conditions of intolerance to certain substances.
Autoimmune diseases. A generalized medical term for pathologies that are based on an excessive reaction of the immune system to the body’s own tissue elements (fragments). That is, the immune system recognizes these elements of the body as foreign and triggers a chain of defensive reactions, leading to severe inflammation and pathologies of various internal organs.
Allergic reactions and autoimmune pathologies can manifest themselves on the oral mucosa and the generalized term allergic stomatitis .
Unfortunately, the relative number of patients with symptoms of allergic stomatitis has recently increased. This is due not only to the fact that the ecology of the external environment is deteriorating or new potentially allergenic components appear in food products. It is believed that a significant contribution is made by the emergence of new and diverse materials used in dental treatment - filling materials, materials for dental crowns and dentures, for the manufacture of braces and implants, various mouth rinses, etc. At the same time, new materials often do not go through the research stage for the risk of allergic reactions. allergic stomatitis may appear and children.
Content:
- Description of the disease
- Manifestations of the disease
- How does allergic stomatitis develop?
- Why does it occur
- Establishing diagnosis
- Fighting the disease
- How to reduce the risk of developing the disease
A dental disease in which the integrity of the oral mucosa is damaged - allergic stomatitis - occurs quite often in medical practice. It comes in different forms, so a person cannot always understand what caused the disease and what factors caused its negative symptoms.
Description of the disease
With the diagnosis described, the oral mucosa is damaged, the tissues become very susceptible to all irritants. The incubation period is long. This means that a lot of time passes from the moment the first signs of allergy appear to the manifestation of the disease itself. Because of this, the patient is unable to track the relationship between the symptoms that bother him.
Allergic stomatitis occurs in both children and adults. More often it is diagnosed in people who live in areas with unfavorable environmental conditions.
Diagnostics
First of all, a visual examination is carried out: the dentist assesses the condition of the mucous membrane, looks for the presence of dentures, fillings and other materials that could become allergens. Then the doctor finds out the time of the first signs of the disease, the patient’s general well-being and possible factors of the disease: heredity, allergies, medication, diet, trips to other countries, contact with animals and insects. If allergic stomatitis is confirmed, tests are performed to clarify the allergen:
- study of the composition of saliva;
- sample from dentures or dental materials;
- immunogram;
- blood and urine tests.
Manifestations of the disease
The disease negatively affects the functioning of the entire body. It doesn’t just cause inflammation of the mucous membranes—it also causes migraines, elevated body temperature, and lethargy. Many people notice dry mouth, severe pain when chewing, which is present even when the integrity of the tissues has not yet been compromised.
Saliva thickens, becomes viscous, more like foam. The gums, tongue, and inner surface of the cheeks may swell. All these symptoms deprive the patient of the opportunity to lead a normal lifestyle.
You shouldn’t wait for the disease to clear up. The sooner her treatment is started, the sooner her health will be normalized.
Erosive-ulcerative stomatitis, cheilitis, glossitis
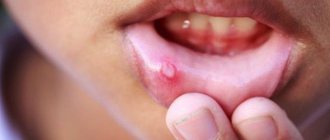
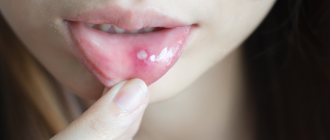
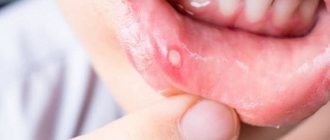
This disease is manifested by hyperemia and swelling of the palate, gums, lips, tongue and cheeks, the appearance of blisters with transparent contents, after opening of which erosions are formed, covered with fibrinous plaque. These symptoms are accompanied by pain, which is aggravated by eating and talking. Weakness, loss of appetite, and increased body temperature up to 38C may appear.
The disease is easily confused with acute herpetic stomatitis, erythema multiforme and pemphigus, so the diagnosis is carried out by an allergist together with a dermatologist.
Treatment consists of discontinuing the intolerable drug and prescribing antihistamines. In severe cases, corticosteroids are prescribed. Local treatment includes painkillers and antiseptic treatment of the oral cavity. It is recommended to eat non-irritating foods and drink plenty of fluids.
How does allergic stomatitis develop?
Dentists distinguish three stages of the disease:
- Primary or catarrhal. A person notices a burning sensation in the mouth, drying out of the mucous membranes. There are no ulcers or plaque yet or they are barely noticeable. If treatment is not started, the resulting ulcers will begin to grow.
- Bullous. Bubbles form on the tissues. There is a cloudy liquid inside them.
- Ulcerative-necrotic. The most dangerous stage in the development of pathology. The pain in the mouth becomes very strong, acute, and does not go away even during rest. The mucous membranes of the mouth swell, turn red, and look inflamed. Numerous ulcers are visible on them, covered with a dense gray coating. If you try to remove the top film, the wound begins to bleed.
You can't start a disease. It is much more difficult to treat the ulcerative-necrotic form of stomatitis than the catarrhal form.
Why does it occur
From the name of the disease it is clear that it is allergic in nature. The disease develops in two cases:
An allergen enters the patient's body. As a result, a pathological response of the immune system develops. We are talking about allergies to pollen, medications, mold, and food.- The tissues of the oral cavity come into direct contact with the allergen. This means that the oral cavity has been treated with something (for example, a medicinal composition, toothpaste, mouthwash) or some kind of dental structure has been installed.
Most often, allergic stomatitis is a consequence of individual intolerance to the materials used by the dentist. Thus, many people are allergic to application solutions, orthodontic appliances, metal braces, and plastic dentures.
An important role in the pathogenesis of the problem is played by advanced caries, chronic tonsillitis, and microorganisms that accumulate under the crowns and cause harm to the mucous membranes. All these are also factors that increase the risk of developing the disease.
Today it has already been proven that people who are diagnosed with allergic stomatitis are more likely to experience:
- inflammation of the stomach, colon mucosa, pancreas;
- disturbance of the gastrointestinal microflora;
- helminthiasis;
- diabetes;
- hyperthyroidism
This is explained by the fact that with these diagnoses, systemic disorders develop in the body, which negatively affect the functioning of the immune system and cause high sensitivity to various types of allergens.
The disease does not always occur in isolation. It is often included in the structure of Lyell's, Reiter's, Stevenson-Johnson syndromes, vasculitis, etc.
Stomatitis
Cold
HIV
Fungus
Scarlet fever
Gastritis
10146 24 September
IMPORTANT!
The information in this section cannot be used for self-diagnosis and self-treatment.
In case of pain or other exacerbation of the disease, diagnostic tests should be prescribed only by the attending physician. To make a diagnosis and properly prescribe treatment, you should contact your doctor. Stomatitis: causes, symptoms, diagnosis and treatment methods.
Definition
Stomatitis is a collective name for diseases of the oral mucosa, manifested by its redness, swelling with the formation of areas of erosion, ulcers or blistering rashes. Stomatitis affects approximately 20% of the population, most often children. Stomatitis can be either an independent disease or a complication or manifestation of other diseases (for example, scarlet fever, influenza, measles, etc.).
Causes of stomatitis
There is no single factor that is the sole cause of oral inflammation. With stomatitis, bacteria or viruses are detected, especially in ulcers on the mucous membrane. However, a diverse microflora is always present in the oral cavity, but stomatitis makes itself felt only when there is a strong additional impact on this microflora.
These impacts include:
- trauma to the mucous membrane caused by overzealous brushing of teeth, rough food, etc.;
- decreased immunity due to colds, vitamin deficiencies, chronic diseases, stress, poor nutrition, as well as more serious diseases (anemia, cancer and autoimmune diseases, HIV);
- entry of a large number of pathogenic microorganisms into the oral cavity through dirty hands, unwashed foods, etc.;
- conditions for the proliferation of pathogenic microflora due to the presence of caries, tartar and plaque, lack of proper teeth cleaning, etc.;
- uncontrolled use of drugs that affect the quantity and quality of saliva and reduce its antimicrobial potential;
- inhibition of normal microflora by antibiotics;
- dehydration of the body with a decrease in the amount of saliva;
- diseases of the gastrointestinal tract (gastritis, pancreatitis, etc.).
Classification of the disease
Due to its occurrence:
- traumatic stomatitis
occurs as a result of the influence of physical (wound, burn from hot food, etc.) or chemical (burn of the oral mucosa with caustic substances, etc.) factors on the mucous membrane; - infectious stomatitis
occurs as a result of a viral, bacterial or fungal infection; - specific stomatitis
occurs as a result of a specific infection (tuberculosis, syphilis); this group includes radiation, drug, and stomatitis due to occupational diseases; - symptomatic stomatitis
develops against the background of diseases of the gastrointestinal tract, cardiovascular, nervous, endocrine systems, and blood diseases; - allergic stomatitis
develops upon contact with allergens.
According to the clinical picture:
- catarrhal stomatitis;
- ulcerative stomatitis;
- aphthous stomatitis.
With the flow:
- spicy;
- chronic.
There are stomatitis associated with dental problems - for example, denture stomatitis occurs due to damage to the mucous membrane by dental structures, due to poor care of removable dentures, and the patient’s failure to comply with oral hygiene.
Symptoms of stomatitis
In children, the disease is more severe than in adults: body temperature may rise significantly and intoxication may be present.
In adults, oral stomatitis, as a rule, is not accompanied by fever, except in cases of deep damage to the mucous membranes in the ulcerative form of the disease.
The most common is catarrhal stomatitis, which is characterized by inflammation of the oral mucosa without the formation of deep defects (ulcers). For those around you, catarrhal stomatitis manifests itself as “stale breath”, for the patient himself – pain, swelling and redness of the mucous membrane. Gingival papillae are easily injured and bleed.
In persons with pathologies of the gastrointestinal tract, as well as with inadequate treatment, catarrhal stomatitis tends to progress to the next stage - ulcerative with the formation of defects throughout the entire depth of the mucous membrane. It is accompanied by an unpleasant odor from the mouth, even putrefactive, the ulcers are covered with a gray coating, and eating any food leads to increased pain. Ulcerative stomatitis is more severe than catarrhal stomatitis and can cause a slight increase in temperature and enlargement of regional lymph nodes.
Aphthous stomatitis manifests itself in the form of small (3-5 mm) single or multiple defects of the mucous membrane of an oval or round shape, surrounded by a thin bright red border and covered with a yellow-gray fibrin coating. Aphthae do not form simultaneously, so you can see different stages of their development. Healing of aphthae begins after the fibrin plaque peels off on its own and ends with the complete disappearance of the defect.
Allergic stomatitis in the mouth occurs against the background of an exacerbation of the underlying disease - allergies. Increased sensitivity of the body can occur to food, medications, pollen, animal hair, cosmetics and care products, and even clothing. Most often, stomatitis is provoked by toothpastes that contain flavorings and chemical components.
Among viral stomatitis, the most common is herpetic stomatitis, which worsens against the background of ARVI. The disease begins with general malaise and lasts 7-10 days.
The oral mucosa becomes red and swollen, and regional lymph nodes become enlarged. After a few days, a blistering rash appears on the tongue and inner surface of the cheeks, and inside the rash there is a translucent liquid. After the bubbles open, small erosions appear, which are covered with a yellowish film.
Diagnosis of the disease
Adequate treatment of stomatitis can be prescribed by determining what caused it - bacteria, fungi or viruses.
If a fungal infection is suspected and to assess the effectiveness of therapy,
Candida albicans
in an oropharyngeal scraping and culture is performed for yeast-like fungi of the genus
Candida
and
Cryptococcus to determine sensitivity to antifungal drugs.
Establishing diagnosis
If there is a suspicion that the patient has allergic stomatitis, he must be examined by a dentist. If necessary, allergists, immunologists, dermatologists, endocrinologists, gastroenterologists, rheumatologists and other specialized specialists are involved in the diagnosis. The attending physician must collect a detailed medical history to understand what caused the disorder and what substance acts as an allergen.
During an examination of the oral cavity, the dentist observes reddened and swollen mucous membranes. In some places, round ulcers are visible on it, covered with a white or gray coating. Saliva is usually very thick.
The specialist pays attention to the condition of the existing prostheses and finds out how long ago they were installed. To study the electrochemical processes occurring in the oral cavity, a saliva test is taken from the patient. It is important to determine the pH of biological material and evaluate the content of microelements in it. Allergy diagnostics involves conducting special tests - skin tests, provocative tests, etc.
If allergic stomatitis is suspected, it is important to differentiate it from a deficiency of vitamins C and B, herpes, candidiasis, leukemia, and HIV. With all these diagnoses, changes in the structure of the oral mucosa are also observed.
Features of treatment
As is often the case with diseases that are at the intersection of several areas of medicine, inflammatory lesions of the oral mucosa are one of the least studied areas of dentistry. Therefore, several specialists can be involved in the treatment of stomatitis in children in the mouth: pediatrician, dentist, dermatologist, immunologist-allergist, otolaryngologist, etc. This is especially convenient when you go to a multidisciplinary clinic.
Self-medication of stomatitis is unacceptable, and although it is now easy to find ready-made treatment regimens and folk recipes, it is important not to experiment with the baby’s health.
Conservative treatment is mainly used, which involves treating the underlying cause of the disease. Your doctor may prescribe the following medications:
- antibacterial drugs (systemic and local in the form of ointments): for bacterial inflammation;
- antiviral agents for herpes and other types of viral stomatitis;
- antifungal drugs for fungal diseases;
- antihistamines - both for allergic origin of stomatitis, and as part of complex therapy to reduce swelling and itching;
- symptomatic drugs - anti-inflammatory, analgesic, antipyretic.
Treatment of candidal stomatitis in infants should be carried out with caution. At the same time, it is important to pay attention to your health; sometimes the cause of such a disease can be insufficient breast hygiene during lactation.
Often, only local remedies are sufficient, but make sure that the entire oral cavity is treated with the rinse - inflammatory agents can be found on the entire surface of the mucous membranes. Healing applications can be used to a limited extent, only on areas of inflammation.
Treatment of stomatitis of any kind in children involves strict adherence to a diet. The diet should be gentle, it is important to avoid salty, spicy, sour foods and drinks, serve the child warm meals, and limit the consumption of sweets.
If traumatic stomatitis occurs, the doctor will prescribe medications to speed up healing. However, it is very important to prevent re-injury. If it was caused by sharp edges of a tooth or filling, this cause should be eliminated. The doctor will suggest grinding off the filling or replacing it, and will also choose the appropriate option for restoring the shape of the crown in case of chips and cracks.
Fighting the disease
What therapeutic regimen the doctor will offer the patient depends on the cause of the disease and the type of provoking factor. The first thing to do is to completely eliminate contact with the allergen. But to do this, you must first establish what exactly this allergen is. If there is no answer to this question, the patient is asked:
- stop taking medications he was previously using;
- follow a strict diet;
- change your toothbrush and toothpaste;
- stop wearing dentures.
In this way, the doctor tries to eliminate the influence of the most common allergens.
Drug therapy involves the patient taking antihistamines. They are always used for allergies. The use of vitamin-mineral complexes is also indicated. It is especially important that they contain folic, nicotinic and ascorbic acid, and B vitamins.
Affected areas should be treated regularly:
- special dental anesthetics;
- corticosteroid gels;
- enzyme compounds;
- drugs that accelerate regenerative processes.
If stomatitis is a consequence of recent dental treatment, you should consult a dentist again as soon as possible. It is possible that you will have to replace the installed fillings and crowns.
Among the folk methods that are effective for stomatitis, rinsing with cabbage juice, aloe infusion, diluted sea buckthorn oil, and chamomile decoction help. You can also apply grated raw potatoes to the wounds.
Treatment of allergic stomatitis in adults and children is carried out according to the same scheme. The only difference is in the medications prescribed: not all formulations for adults are suitable for children, and vice versa.
Catarrhal and catarrhal-hemorrhagic stomatitis, cheilitis, glossitis
This is the mildest form of drug allergy. It is manifested by itching, burning, impaired taste sensitivity, dryness and pain when eating.
Clinical symptoms: hyperemia, swelling of the mucous membrane, as indicated by tooth marks on the lateral surfaces of the tongue and cheeks. Differential diagnosis is carried out with similar changes in the oral mucosa in cases of hypovitaminosis C, B, gastrointestinal diseases, infectious and fungal infections.
For this disease, both local treatment is used in the form of rinsing with antiseptic agents and taking painkillers, as well as general treatment: withdrawal of allergen medication, antihistamines (Diphenhydramine, Diprazin, Suprastin, Tavegil), calcium supplements. It is recommended to drink plenty of fluids and eat foods that do not irritate the mucous membranes.
How to reduce the risk of developing the disease
If stomatitis has already occurred, the likelihood of it reoccurring is very high. To avoid illness, you should follow the recommendations:
Pay maximum attention to oral hygiene. It is unacceptable to brush your teeth only occasionally. This should be done in the morning after meals and in the evening before bed. After each snack, it is advisable to rinse your mouth with warm water. To prevent plaque from accumulating in the interdental spaces, they need to be cleaned daily with dental floss or an irrigator.- Strengthen immunity. During the cold season, you need to take a vitamin-mineral complex. Proper nutrition is of particular importance. The diet should be enriched with fresh fruits and vegetables.
- Give up bad eating habits. You need to stop consuming large amounts of spices and alcohol.
- Combine medications wisely. If you need to take antibiotics for a long time, it is advisable to include antihistamines in the course - drugs that reduce the likelihood of developing allergic reactions.
- Have professional oral hygiene every year. This is a general strengthening measure. It keeps teeth and gums healthy for many years.
Regular visits to the dentist allow you to detect all dental diseases at the earliest stages. Therefore, even if nothing bothers you, do not forget to visit your doctor once every six months.
Prevention
If a patient once experiences allergic stomatitis, there is a high probability of it developing again. To prevent pathology, you need to pay attention to the following points.
- Immunity.
To strengthen the immune system and general health, it is recommended to take a course of comprehensive vitamin intake. - Nutrition.
It is better to exclude allergenic foods and hot spices from food and create a balanced menu. - Medicines.
When taking strong medications, especially antibiotics, it is necessary to include antihistamines, that is, antiallergic agents, in the list of medications. - Oral care.
If a toothpaste, brush or mouthwash causes discomfort, irritation or itching, you need to change the products yourself or choose the right ones together with your dentist.
The risk of developing allergic stomatitis and other diseases is minimal if you visit the dentist every six months for the prevention and timely treatment of pathologies in the early stages!