Dentist-therapist
Spivak
(Therapist) Evgenia Ivanovna
Experience 28 years
Dentist
Make an appointment
Stomatitis is a characteristic inflammation of the oral mucosa. More common in children, this is due to the habit of not washing their hands and “tasting” surrounding objects. It can act as an independent disease or develop against the background of mechanical damage, infections or dental diseases. Manifestations of pathology are different: from small ulcers to large inflammations over the entire surface of the mucosa. Provided that you seek medical help in a timely manner and take a course of medication under the supervision of a doctor, it can be completely cured.
What is stomatitis?
Stomatitis, which means “mouth” in ancient Greek, is the most common name for a group of diseases of the oral mucosa. The disease should not be confused with glossitis (damage to the tongue), cheilitis (damage to the lips) and palatinitis (damage to the palate). Stomatitis is not contagious, but almost every person has directly or indirectly encountered one or another type of the disease. Once you have been ill, the chance of recurrence of the disease is very high.
Correctly diagnosing stomatitis is difficult. The doctor often assesses the situation only visually - in medicine there are no special tests for this disease. The difficulty of diagnosing stomatitis also lies in the fact that it can be a symptom of more serious diseases.
Causes of stomatitis
The mechanism of stomatitis, unfortunately, has not yet been fully identified, so there are many causes of the disease:
- microorganisms that cause infection, acting directly on the oral mucosa;
- diseases of the gastrointestinal tract;
- diseases of the cardiovascular system;
- general weakening of the immune system;
- avitaminosis;
- metabolic disorders;
- nervous disorders;
- malignant tumors;
- hormonal fluctuations;
- various injuries in the form of abrasions of the oral mucosa;
- anemia;
- heredity.
Among the causes of stomatitis there are also local factors. Elementary lack of oral hygiene, caries, dysbacteriosis, poorly made or poorly installed dentures, the consequences of using medications, nicotine and alcohol consumption, as well as allergic reactions to products. Of particular note is the use of toothpastes containing sodium lauryl sulfate. Various studies have proven that they provoke the occurrence of stomatitis and its exacerbation.
Diagnostics
The diagnosis of “allergic stomatitis” is made by a dentist based on an examination of the oral cavity and questioning the patient about underlying diseases and medication use. The dentist clarifies the clinical picture of the disease.
The doctor must conduct a comprehensive examination and diagnosis:
- removable and fixed prostheses;
- braces;
- filling
To clarify the clinical picture of the disease, the specialist refers the patient for a comprehensive blood and urine test and an immunogram to assess the state of the immune system. If necessary, the doctor sends the patient for the following studies:
- determination of the acidity level and composition of saliva;
- identification of the activity of enzymes contained in saliva;
- leukopenic test;
- provocative tests with removal and subsequent installation of prostheses.
An integrated approach to diagnosing allergic stomatitis will allow you to quickly find out the cause of the negative reaction, eliminate it and begin effective treatment.
Symptoms of stomatitis
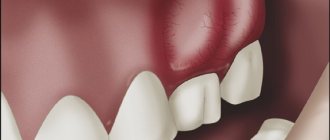
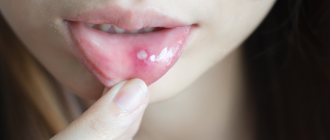
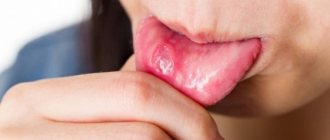
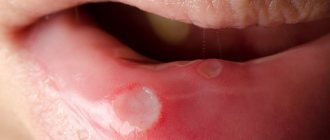
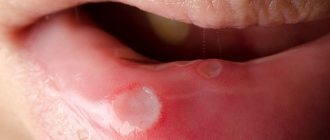
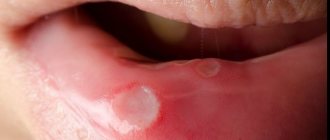
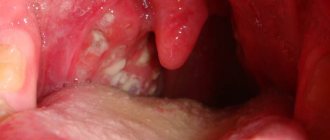
Light redness of the oral mucosa is the first symptom of stomatitis. Over time, they swell and a burning sensation appears. If treatment is not started at this stage, the redness is replaced by small oval or round ulcers, grayish or white, with a red halo and a film on top. Moreover, the tissue around them looks absolutely healthy. Mouth ulcers are very painful and make eating difficult. They appear on the inner surface of the cheeks and lips, under the tongue. In most cases, mild stomatitis manifests itself as one ulcer.
The appearance of several ulcers of larger size and depth, which sometimes merge into one, are signs of more severe forms of stomatitis. The appearance of ulcers is accompanied by fever, inflammation of the lymph nodes, general deterioration of health, headache, loss of appetite and constipation. Acute stomatitis is accompanied by severe pain in the mouth, which interferes with eating and speaking. In addition, there may be excessive salivation, a coating on the tongue, a bright red mouth, irritability, and vomiting after eating.
Can stomatitis be a side effect after taking medications?
Rare, but still acceptable causes of stomatitis also include taking certain medications.
Some antibiotics, diuretics, and oral contraceptives affect the condition of the oral mucosa, causing increased dryness and other complications. If your mouth becomes very dry, cracks and ulcers may occur.
Types of stomatitis
There are many types of oral stomatitis.
Catarrhal stomatitis
The most common type of stomatitis. With this unpleasant disease, the oral mucosa becomes swollen, painful, hyperemic, and may be covered with a white or yellow coating. There is an increased secretion of saliva. All this may be accompanied by bleeding gums and bad breath. The causes are local factors: poor hygiene, caries, tartar, oral candidiasis. Catarrhal stomatitis also occurs as a result of diseases of the gastrointestinal tract and worms.
Ulcerative stomatitis
A more severe disease than catarrhal disease. It can develop independently or be an advanced form of catarrhal stomatitis. Most often it develops in people suffering from gastric ulcers or chronic enteritis, diseases of the cardiovascular system and blood, infections and poisoning. With ulcerative stomatitis, the entire thickness of the mucous membrane is affected, there is an increase in temperature to 37.5 0C, weakness, headache, enlargement and tenderness of the lymph nodes. Eating is accompanied by severe pain.
Aphthous stomatitis
Causes of the disease: gastrointestinal tract, allergic reactions, viral infections, rheumatism, and heredity. Aphthous stomatitis has symptoms:
- the appearance on the oral mucosa of single or multiple aphthae - small ulcers (3 - 5 millimeters) of gray-white color with a narrow red rim;
- bad feeling;
- increased temperature and pain of ulcerative lesions.
The disease can have an acute form or occur chronically with periods of exacerbation and remission, the so-called chronic recurrent aphthous stomatitis.
Candidal stomatitis
It is a fungal disease that most often appears in young children (stomatitis in children) and the elderly. This type of stomatitis is caused by a fungus (usually the Candida genus) and develops mainly when the body’s immune forces decrease, as a result of long-term treatment with strong antibacterial drugs, as well as against the background of another chronic disease. Candidal stomatitis has the following symptoms:
- burning sensation in the mouth and larynx,
- white coating on the tongue and mouth,
- hyperemia and bleeding of the mucous membrane,
- bad taste in the mouth or loss of taste.
This type of stomatitis is considered contagious and can be transmitted both through household and sexual contact.
Herpetic or herpes stomatitis
Occurs in both adults and children. It is caused by the herpes simplex virus and can be acute or chronic. Symptoms of herpetic stomatitis:
- in mild cases, small blisters appear, resembling aphthae;
- the severe form is characterized by multiple rashes on the mucous membrane;
- swelling and inflammation of the lining of the oral cavity;
- increased salivation;
- general malaise;
- toxicosis;
- elevated temperature;
- enlarged lymph nodes;
- burning sensation and pain when eating.
The peculiarity of herpetic stomatitis is that the herpes virus remains in the body forever.
Allergic stomatitis also occurs; read more about the disease in the article.
Allergic stomatitis
It is an allergic disease that can occur in both adults and children. Its etiology is different: if in childhood the allergen is most often food products introduced into the child’s diet for the first time, then in adult patients the triggering mechanism for the pathological reaction may be weakening of the immune system due to the use of certain medications, rejection of dentures or advanced inflammatory processes in the oral cavity.
The characteristic signs of allergic stomatitis are:
- itching in the mouth, increasing after eating;
- severe swelling of the oral mucosa;
- secretion of a large amount of thick saliva;
- hyperthermia;
- unbearable pain;
- bad breath.
For the treatment of allergic stomatitis, in addition to visiting a dentist, consultation with an immunologist and an infectious disease specialist is recommended.
How to prevent relapse?
If once stomatitis has already made itself felt, it is worth making some changes in your life that will help avoid relapse:
- do not put off dental treatment until later;
- do not ignore nasopharyngeal diseases;
- treat gastrointestinal problems in a timely manner;
- supplement your oral hygiene with a rinse and irrigator;
- Make a habit of eating vegetables or fruits at every meal;
- take a course of multivitamins twice a year;
- avoid injuring the oral mucosa with hot and cold foods;
- take care not only of your physical, but also of your mental health: get enough sleep, rest on time, pamper yourself.
It is especially important if you are prone to stomatitis to choose a competent dentist. At the first visit, you need to tell him about past problems so that the doctor can prevent the development of the disease. For example, be as careful as possible when removing tartar or immediately prescribe gum treatment with Metrogil Denta gel when installing a prosthesis.
Author: Elena Grunina Dentist-therapist, endodontist. Work experience more than 9 years.
The information is for reference only. Before treatment, consultation with a doctor is necessary.
How to treat stomatitis?
Any treatment for stomatitis begins with a professional hygienic cleaning procedure, during which tartar and soft plaque are removed. Almost any dental clinic in Moscow provides a similar service. Teeth affected by caries are treated. The mucous membrane is treated with antiseptic rinses. During the day, rinse the mouth with a warm solution of chamomile or calendula decoction. With timely treatment, catarrhal stomatitis disappears in 5–10 days. For ulcerative or aphthous stomatitis, local treatment is combined with general treatment. In addition to professional oral hygiene, antiseptic procedures are carried out in the clinic where stomatitis is treated.
If the presence of herpetic stomatitis is suspected, additional antiviral therapy is carried out. In case of oral candidiasis, treatment is prescribed with antifungal drugs. If the cause of stomatitis is some other disease, for example, the stomach or intestines, then it is necessary to begin to treat the root cause. During the treatment process, you should definitely follow a diet limiting spicy, hot, cold, sour and rough foods. A side effect of taking medications can be a green coating on the tongue.
Possible complications
If stomatitis in the mouth is left untreated, it will certainly lead to negative consequences, from gum inflammation to tooth loss. That is why it is extremely important when treating stomatitis to strictly adhere to the recommendations given by your dentist. The list of major potential complications includes the following diseases.
- Chronic stomatitis.
Statistically, this is the most common complication. An untreated inflammatory process becomes chronic and recurrent, which means that an infectious focus will always be present in the body. - Appearance of scars.
A symptom such as bleeding gums can be a manifestation of many diseases, but with stomatitis, due to constant non-healing cracks in the oral cavity, scar tissue forms, which in the future may not allow the patient to open his mouth wide. - Laryngitis.
If the infection spreads up the respiratory tract, the patient's voice becomes hoarse and a cough appears. - Vision problems.
With advanced herpetic stomatitis, the target of damage becomes not only the gums, but also the mucous membranes of other organs. Most often, these are the eyes and genitals. - Loss of teeth.
The most dangerous complication of stomatitis. The main threat is the fact that the destructive process can last for many years and may not be noticeable to the patient at first. First, periodontal disease will develop - serious damage to periodontal tissue. And only then, as a consequence, the teeth will gradually become looser until they fall out.
Allergic stomatitis in children
In children, the disease occurs more often than in adults, and at the same time, a weak and fragile child’s body reacts more sharply to irritants. The baby begins to be capricious, complain of pain in the mouth and, of course, is afraid to go to the dentist.
In no case should parents let a child’s illness take its course, relying on traditional methods of treatment. If the baby suffers from allergic stomatitis, no ointments or rinses will cure him 100% as long as contact with the allergen continues. Sensitive thin mucous membranes easily crack, bleed, and pathogenic microorganisms quickly penetrate into the ulcers.
It is important to take the child to a specialist as soon as possible, explain to him that the doctor will help him get rid of the pain, and begin the examination.
Stomatitis and treatment at home
Treatment of stomatitis at home primarily involves the use of various herbal decoctions and infusions with antiseptic, anti-inflammatory and immunostimulating effects. For example, even doctors recommend rinsing with calendula - it has a strong antimicrobial and anti-inflammatory effect and promotes healing. Chamomile is an excellent antiseptic - it is one of the most popular remedies that is widely used in folk and official medicine.
Stomatitis is treated using folk remedies not only for rinsing, but also for oral administration. For example, rosehip decoction is a real storehouse of vitamins and other substances necessary for the human body. It improves immunity, prevents the development of inflammatory processes, and also helps destroy harmful bacteria. Despite the miraculous power of herbs, it should be remembered that candida and herpetic stomatitis will not be eliminated by such folk treatment, since fungi and viruses are not affected by antiseptic, anti-inflammatory and immune-modifying agents.
How to treat the disease
Therapy involves the use of local and sometimes systemic drugs. The treatment regimen for the disease depends on what type of stomatitis is diagnosed. For this reason, you should not self-medicate, as it may turn out to be useless and the pathology will continue to develop into dangerous conditions.
The exception is mild catarrhal inflammation associated with poor hygiene. It is enough to exclude the cause and rinse your mouth with antiseptics for several days.
Treatment at home for other types should be discussed with your doctor. The use of folk remedies is not contraindicated, but they can only be used as a supplement to the main therapy. Only a dentist can evaluate the appropriateness and harmlessness of a particular prescription.
Effective drugs for adults
To relieve inflammatory processes, combat pathogenic microflora, and relieve pain, rinses, gels, sprays, lozenges, and ointments are prescribed. For severe pain, pain medications can be taken orally. Since treatment must be carried out regularly, it is important to choose a medicine for stomatitis that will be convenient to carry in your purse and use at work.
Popular medicines:
- Chlorophyllipt, Inhalipt, which have an antiseptic effect. Available in the form of sprays. Apply up to 5 times a day for one week. Sprays are convenient to use if there is stomatitis in the palate or throat.
- Solcoseryl accelerates tissue regeneration, restores mucous membranes, and protects against the development of ulcers. The gel is applied several times a day. The course is from 7 to 14 days.
- Cholisal has a detrimental effect on bacteria, relieves inflammation, and improves tissue healing. The gel is used three times a day for at least a week. An analogue of the drug is Kamistad. Excellent help with aphthous, bacterial form of the disease.
- Viferon, Acyclovir are prescribed to patients with a viral infection. Ointment for stomatitis in the mouth is applied to areas of inflammation several times a day. The course of therapy is up to 2 weeks.
- Lidocaine Asept, Lidochlor are used for any form of pathology, since the main purpose is to relieve acute pain. Available in spray form. Can be used up to four times a day, no more than 1 week.
- Lugol kills bacteria, treats ulcers, and relieves inflammatory processes. The oral cavity is treated with a spray 2 - 3 times a day.
- Miconazole and Nystatin are prescribed for fungal infections. In severe cases of the disease, the ointment is used in combination with systemic medications. Apply to affected areas 2 to 4 times a day.
Any medication for stomatitis must be prescribed by a doctor. The symptoms of the varieties of the disease are similar and it is impossible to independently understand the cause of the inflammatory reactions.
What can you rinse your mouth with?
To treat pathology, you can use pharmaceutical drugs aimed at destroying bacteria, reducing inflammation and healing tissue.
Medicinal solutions that can be bought at the pharmacy:
- Aqualor with sea salt;
- Stomatofit, Dr. Theiss Sage based on sage;
- Romazulan with chamomile extract;
- Chlorhexidine (pre-diluted with water).
Decoctions and infusions for rinsing are easy to prepare at home from chamomile, calendula, aloe juice, sea buckthorn, linden flowers and other medicinal plants. A solution of salt and soda helps a lot.
Prevention of stomatitis
The basis for the prevention of stomatitis is compliance with the rules of oral hygiene. Brushing your teeth twice a day with an ultrasonic brush and visiting a hygienist every six months are mandatory. It is important to monitor the general condition of your teeth. Wearing braces or dentures will require special attention, as they can injure the oral mucosa.
To prevent stomatitis, it is very important to be careful about your diet. Using special tests, it is recommended to identify and exclude foods that cause allergies from the diet. You should not eat foods that have a traumatic or irritating effect on the oral mucosa: crispy, salty, hot and spicy foods. Tomato and orange juices and alcohol are not recommended. The diet must be sufficiently balanced, since a lack of vitamins and microelements can cause an attack of the disease. Remember that stomatitis is always recurrent, that is, it occurs periodically during periods of general weakening of the body.
If you have had stomatitis at least once in your life, there will always be a risk of it occurring again. Therefore, prevention comes to the fore. Avoid bad habits, stick to a diet, try not to be nervous and, of course, maintain oral hygiene!