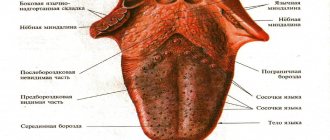
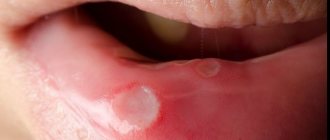
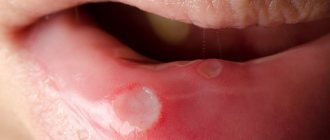
The candida fungus, which causes damage to the mucous membrane of the genital organs in men and women, can also actively multiply in the mouth, then candidiasis or oral thrush is formed in adults.
The disease is not uncommon and brings a lot of suffering to patients, sharply reducing the quality of life and disrupting the process of eating.
There are a large number of different stomatitis, that is, inflammation of the oral mucosa, bacterial, viral and fungal in nature. Sometimes mixed. The signs of these diseases are very similar, but the correct treatment tactics and recovery depend on an accurate determination of the nature of the disease. In this article we want to tell you what exactly oral thrush is in adults, the symptoms and treatment of this fungal infection of the oral cavity.
In general, Candida albicans is present in small quantities on almost all mucous membranes, including the oral cavity. But being in a balanced ratio with other representatives of microflora, it does not cause any diseases. That is, thrush in the mouth of adults will not arise just like that, without apparent reasons.
Who's at risk
First of all, these are people who have the following unfavorable factors:
- Weakened immunity.
Defects in immune defense are the main factor predisposing to the occurrence of mycoses (fungal infections)1,2,4. The increase in their incidence in all countries of the world is due, first of all, to various types of conditions accompanied by weakened immunity1,[3]. It is not for nothing that “thrush” is called “the disease of the sick”1. Among its reasons:
- severe general diseases, for example, infectious2,3;
- cancer accompanied by sudden weight loss, lack of vitamins and microelements, requiring radiation and chemotherapy2,3;
- congenital and acquired forms of immunodeficiency, including AIDS2,3;
- endocrine disorders, for example, diabetes mellitus2,3.
- Dental diseases.
- Inflammatory , such as caries and its complications, gingivitis, periodontitis, periodontal disease and others2. The huge number of bacteria present during inflammation weakens the immune system and contributes to the proliferation of fungal microflora2. A diseased tooth with a carious cavity “infested” with microbes or a periodontal pocket filled with pus may well provoke the development of “thrush”3,[4].
- Non-inflammatory , which change the structure of the oral mucosa, for example, folded tongue and leukoplakia4. It is easier for fungi to attach to a damaged surface than to a healthy one.
- Constant dry mouth.
- Insufficient saliva (xerostomia), associated with a variety of problems, contributes to the development of oral mycosis4. Saliva contains many enzymes and antibodies that protect the mucous membrane from the action of microbes4. If there is little saliva, it dries out, its protection is weakened, which creates favorable conditions for the development of other infections.
- Defects in oral hygiene.
- Insufficient care . Problems more often arise in those who rarely brush their teeth and ignore the care of their tongue, interdental spaces and dentures4.
- Injuries . Sometimes the cause of an “outbreak” of oral mycosis is a too hard toothbrush or rough manipulation of dental floss and toothpicks. Injured gums are easy prey for fungi2.3,4.
- Incorrect use of removable dentures.
- Poorly customized removable dentures can rub the gums3,4, making them accessible to germs.
- No night break in using prostheses4. The gum located under the prosthesis is poorly enriched with blood, it lacks oxygen, it is not washed with saliva - this predisposes to the development of infection4.
- Improper care of dentures. Artificial teeth need care just as much as your own. Deprived of attention, they become covered with a thin film of various microbes, which then “attack” the gums.
- Age.
- Most often, doctors find “ thrush” in the mouth of infants and the elderly4. The reason for this is the imperfections of the immune system, which create favorable conditions for the proliferation of pathogenic microflora1,4,[5]. In addition, in childhood, dietary habits affect, and in old age – constant dry mouth and lack of teeth, forcing you to wear dentures1,5.
- Medicines
- Antibiotics. They kill not only pathogenic microbes, but also beneficial ones, thereby disturbing the balance of microflora and creating conditions for mycoses to flourish1,2.
- Drugs that inhibit cell proliferation (cytostatics). They interfere with the renewal of surface mucosal cells and disrupt local and general defense mechanisms against infections1,2.
- Immunosuppressive medications, which are prescribed when immune responses need to be suppressed, such as during transplantation1,2.
- Inhaled corticosteroids, which are used in the treatment of bronchial asthma and, due to their side effects, increase the susceptibility of the mucous membrane to infections2,[6].
- Unbalanced diet
- Lack of iron, vitamins C and B12, and folic acid1 in the diet, which leads to decreased immunity.
- Excess carbohydrates1,2. Excessive consumption of sweets, flour products, sweet fruits, starchy vegetables and other foods containing large amounts of simple carbohydrates contributes to the appearance of thrush in adults and children1,2.
Up to contents
How does the infection manifest and why is it dangerous?
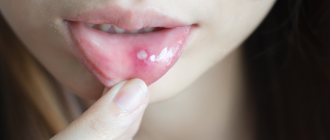
The most striking symptom of oral candidiasis is a white, loose coating on the mucous membrane. It mainly covers the tongue, cheeks, and may affect the gums and palate. Plaque can be easily scraped out; the tissue underneath is prone to redness and may bleed. Other signs of the disease include:
- unpleasant taste;
- dry mouth;
- burning;
- the appearance of cracks in the corners of the lips;
- difficulty or painful swallowing;
- unpleasant sensations with habitual movements of the tongue.
Candidiasis can be acute or chronic. In most cases, it is the acute form that manifests itself; the chronic form is typical for carriers of HIV infections and smokers. Depending on the degree and form of the disease, other symptoms may be observed, so even if one or two appear, you should immediately contact your dentist.
What does thrush look like in the mouth - its symptoms in adults
After Candida attaches to the mucous membrane, they multiply and “grow” deep into it2, causing inflammation, swelling and redness. There is a feeling of a “scalded mouth” and discomfort when eating and swallowing. There may be a change in taste and the appearance of a metallic, sour, salty or bitter taste1.
The proliferation of the fungus leads to the appearance of small white spots on the gums, tongue, inner surface of the cheeks and palate, reminiscent of curdled milk or grains of semolina porridge. Increasing in size, the “grains” turn into plaques, which, in turn, merge to form solid white films.
If plaques and films are removed with a spatula or a cotton swab (this does not require additional effort), then a bright red inflamed, eroded mucous membrane is revealed underneath them.
Oral mycosis can spread to the red border of the lips , causing redness, dryness and peeling. Seizures appear in the corners of the mouth: the skin becomes inflamed, covered with grayish-white scales and cracks5.
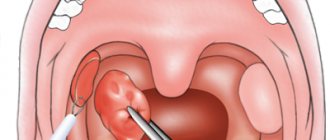
If candidiasis is not treated at this stage, the fungi “spread” to the tongue and pharyngeal tonsils.
When the tongue is damaged, glossitis develops - the tongue swells, its papillae are smoothed out, a characteristic white coating appears on its back and lateral surfaces1 - and when the pharyngeal tonsils are damaged, a sore throat occurs.
A sore throat caused by fungal microflora is very different from normal. With obvious inflammation of the tonsils and the presence of white films and plugs on them, there is no temperature or pain when swallowing, and the submandibular lymph nodes remain of normal size1.
Candidiasis can spread further - affecting the respiratory tract, causing pneumonia and blood poisoning, so it is important to stop the process at the very beginning.
Up to contents
Features of “thrush” in the mouth in children of the first year of life
Mycoses in children, and very young ones at that, are not that uncommon. According to statistics, the first illness of a newborn in 33% of cases is associated with Candida fungi5. Moreover, they mainly affect the skin and tissues of the oral cavity5.
Why does thrush appear in the mouth of a child under one year old?
Mycotic stomatitis, or fungal inflammation of the oral mucosa, is the most common form of mycosis in children under one year of age1.5. How do mushrooms get into a baby’s mouth and why do they take root there? There are many reasons for this.
- Infection during childbirth.
During childbirth, the fetus comes into contact with the microflora of the woman’s vagina. If the mother suffered from vaginal candidiasis before giving birth and did not undergo the necessary course of treatment, the baby has every chance of inheriting a large amount of the causative agent of this disease1.5, which is a big burden for the immature immune system. According to statistics, on the first day of life, Candida fungi are found in the oral stool of 25-40% of newborns5.
- Unsanitary conditions.
Infection is possible due to violation of the rules of care for the newborn and defects in the hygiene of the nursing mother herself1,5. The infection is transmitted through dirty nipples and hands during feeding, through toys, nipples, dishes and linen.
- Imperfect immunity1, 5.
In a baby under one year old, the immune system is only “gaining experience”, because in the womb it did not come into contact with the infection and therefore “did not learn” to fight it.
- Prematurity and illness.
Candida can only harm a weakened body. The best conditions for their development are created if the birth occurs before term, the fetus is premature and/or has developmental defects or congenital diseases5.
- Nutritional features.
The threat is posed by regurgitation, the habit of putting the baby to bed with a bottle of milk and feeding with sweet artificial formulas. If milk remains in the mouth, which also contains a large amount of sugar, it becomes an ideal breeding ground for mushrooms.
- Features of salivation.
Due to physiological characteristics, the salivary glands of infants produce little saliva1 - they simply do not need it, since food is already liquid. At the same time, saliva has antifungal activity, and when there is little of it, the likelihood of oral thrush in a newborn increases1,5.
What does oral candidiasis look like in children?
The symptoms are the same as in adults: first, white “grains” appear on the mucous membrane, then “clumps” resembling curdled milk, and white films1. The difference is that the process is almost always accompanied by severe tissue swelling and the formation of numerous painful ulcers on the oral mucosa and tongue1,5. Therefore, due to oral thrush, infants often refuse to eat5.
In children, a fungal infection can affect not only the tonsils (tonsillitis), but also the pharynx (pharyngitis) and larynx (laryngitis). If the larynx is affected, the baby's voice becomes hoarse and low, and there is a risk of swelling of the airways and breathing problems1, 5.
Up to contents
Examination of patients with oral candidiasis
Laboratory diagnosis of oral thrush is not difficult, but for some reason many doctors do not perform it in full.
First of all, films, plaque and scrapings from erosions and ulcers are taken for analysis.
The resulting material is examined microscopically, detecting elements of yeast fungi in it, as well as by PCR and inoculation.
The OCR for candida helps to determine the type of fungus and its quantity in a fairly short time - within 1 day. For erosions, it is also recommended to take an analysis for Treponema pallidum, the causative agent of syphilis, and herpes viruses, which cause similar symptoms.
Sowing will help to find out which antimycotics candida is sensitive to and which accompanying microflora is involved in the inflammatory process. It is done within 5–7 days. Although a variety of it has now appeared - spectral analysis, which allows you to get results in 3 days, its cost is much higher.
Blood tests are also necessary to evaluate a patient with oral thrush. They will help identify diabetes, syphilis, HIV and immune problems.
Also, this diagnosis is needed to determine the condition of the liver and kidneys, which will have to deal with the processing of antifungal drugs during the treatment of thrush. If the function of these organs is impaired, the selection of drugs for drug therapy is complicated, because they have a pronounced effect on the liver and kidneys. This diagnosis is no less important than scrapings from rashes.
If signs of thrush in adults occur after sexual intercourse, then the venereologist takes tests from the oropharynx, erosions, ulcers, and tongue for STIs - sexually transmitted infections. PCR diagnostics are also mainly used. The presence of chlamydia, gonococcus, mycoplasma, gardnerella, and HPV, which can also affect the oral mucosa, is determined.
If the level of glucose in the blood increases, a consultation with an endocrinologist is prescribed. Because without normalizing high sugar levels, it is simply impossible to cure oral thrush, no matter what methods and medications the doctor used.
The patient may be referred to an immunologist if serious abnormalities in the immune status are detected. Sometimes, without correcting the immune system, it is also impossible to cope with candidiasis.
Only with all this data will the doctor prescribe the correct treatment. Without a complete diagnosis, there is a risk of transition to a chronic form of the disease, the success of treatment of which is already more questionable than a fresh infection.
Diagnosis of oral mycosis
Most often the diagnosis is obvious. However, in difficult situations, for example, in the presence of complications or individual intolerance to certain drugs, to confirm it, microscopic and cultural analysis of scrapings from the surface of the mucous membrane is used to determine the sensitivity of the microflora to antifungal drugs. Moreover, the mere presence of Candida threads in scrapings from the oral cavity is not always enough to make a diagnosis - fungi can be present in the mouth, but not cause any diseases. In such a situation, quantitative assessment is important, that is, counting the pathogen cells, and increasing their number when re-analyzed after 2-3 days.
Up to contents
How and with what to treat thrush in the mouth
Since candidiasis often develops as a secondary disease1, treatment of oral thrush requires an individual approach. What do we have to do?
1. Eliminate the factors that contributed to the appearance of oral mycosis
To do this you need:
- cure diseased teeth and gums, relieve exacerbation of chronic tonsillitis, pharyngitis;
- replace old “outdated” removable dentures with new ones, follow the rules for using and processing dentures;
- every time after using inhalers with steroid drugs (for bronchial asthma), rinse the mouth and gargle with water6;
- take antibiotics only as prescribed by a doctor;
- use toothbrushes with soft bristles, toothpastes, and mouthwashes with an anti-inflammatory effect1;
- follow the rules of caring for a newborn and feeding hygiene (if the disease manifests itself in an infant);
- use formulas that do not contain sugar for artificial feeding of a newborn.
2.Keep a diet
Meals include:
- limiting the daily intake of simple carbohydrates: sweets, flour products, potatoes, rice, legumes, boiled beets and carrots, sweet fruits and dried fruits;
- supplementing the diet with fresh vegetables with a lot of fiber, which contribute to the formation of normal microflora in the intestines and the formation of immunity9;
- consumption of sour berries and lactic acid products, which, due to their acid content, hinder the spread of fungi1;
- taking vitamins1 necessary for the normal functioning of the immune system;
- eating enough easily digestible meat and eggs for the normal functioning of the immune system.
3. Carry out local treatment
For oral thrush in both adults and children, treatment may include topical use of drugs with antifungal activity. Moreover, if the fungus affects only the oral cavity, local therapy may be sufficient5 to cope with the problem.
To treat the oral mucosa, today it is recommended5 to use hexetidine preparations, for example, HEXORAL® solution and HEXORAL® aerosol .
HEXORAL® with hexethidine:
- is active against biofilms[7] that are resistant to other drugs, and is harmful to fungi of the genus Candida, which cause oral candidiasis;
- has a high safety profile;
- can be used not only in adults, but also in children from 3 years old8;
- eliminates discomfort and relieves pain7;
- lasts for a long time, up to 12 hours[8];
- Available in the form of a solution and an aerosol, for comfortable use in any situation (for fungal laryngitis in children, it is especially convenient to use the aerosol form of the drug)2.
Important: doctors prescribe general antifungal drugs only if local treatment is ineffective and multiple relapses of candidiasis occur against the background of severe immunodeficiency and/or severe concomitant diseases. In these cases, HEXORAL® can be an addition to the main therapy1, 2, 5.
When treating oral thrush in newborns, there is often no need to use systemic antifungal agents1, 2, 5.
Up to contents
Treatment of candidiasis: recommendations for the patient
During treatment, it is recommended not to temporarily use removable dentures. If there is a need to wear removable orthopedic structures every day, it is recommended to regularly treat them with the same antiseptics as the oral cavity. Also, a sick person will have to reconsider his diet. Foods high in carbohydrates, starch and sugar promote the growth of Candida fungus. They create an environment in the oral cavity that is favorable for the proliferation of the pathogen. For a speedy recovery, it is advisable to adhere to a healthy diet and drink plenty of water.
Perform oral hygiene after every meal. Follow all doctor's recommendations, rinse your mouth regularly and use only the medications prescribed by your doctor. If the white coating does not come off from your tongue or cheeks, do not try to remove it yourself. You can injure the mucous membrane of the oral cavity, as a result of which the causative agent of candidiasis will enter the bloodstream and the infection will spread throughout the body.
How to prevent the disease
So, what will help avoid an “outbreak” of fungal infection?
- Careful oral care.
- Solving dental problems and treating common diseases.
- Compliance with the rules of personal hygiene, hygiene of infant feeding and care1.
- Mandatory treatment of the disease during pregnancy and after childbirth1.
- Prophylactic use of antifungal agents, for example, during treatment with antibiotics and immunosuppressive drugs (radiation or chemotherapy)1.
Important: frequent outbreaks and severe cases of candidiasis are a reason to consult a doctor and undergo a full examination. Taking into account the fact that mycoses develop against a background of reduced immunity, they can act as a marker of serious diseases2. According to the World Health Organization, recurrent candidiasis should be a reason for testing for HIV.
Up to contents