Hemangioma occurs in children from the moment of birth, but most often it appears in the first two months of a newborn child’s life, which is extremely frightening for parents. Meanwhile, there is no reason for serious concern: the neoplasm never degenerates into a malignant tumor and does not cause physical pain to the baby. The exception is when the hemangioma is injured (for example, by clothing), which leads to bleeding from the vascular formation and the formation of a wound surface, which can subsequently become infected. This situation requires immediate surgical treatment.
Hemangioma has one positive feature: in children from one year to 2 - 3 years old, the process of invaluation of the hemangioma occurs, that is, it independently decreases in size, until it completely disappears!
Alexander Genrikhovich Dorofeev
Candidate of Medical Sciences, pediatric surgeon, doctor of the highest category at the Scientific Research Institute of National Chemistry and Technology
Description of the disease
Atheroma is one of the relatively harmless tumors due to the fact that it does not transform into a malignant neoplasm.
However, there is a risk of significant increase in size, so medical attention is required in all cases. Teenage children are more likely to experience this problem. Boys and girls get sick about the same. The main reason why parents first turn to a surgeon is the presence of a visually noticeable tumor.
The atheroma itself is a small capsule filled with pasty contents. It is sebum, which, due to blockage of one or more glands, did not come out, but remained in the subcutaneous tissue.
Causes and symptoms of the disease
Currently, medicine cannot yet accurately answer the question of why and how hemangioma appears in a child. According to one theory, somewhere at the stage of angiogenesis (i.e., the formation of blood vessels during intrauterine development) a genetic failure occurs. Among the risk factors that cause the appearance of hemangioma in children, doctors include:
- - premature pregnancy,
- - late first birth,
- — ARVI suffered by a pregnant woman in the 1st trimester,
- - taking various medications during pregnancy,
- - disturbance of placental circulation in the fetus,
- - bad habits of the mother (alcohol and nicotine consumption),
- - living during pregnancy in an area with poor ecology.
Symptoms of atheroma in children
In 80-85% of cases, apart from the visual defect, children do not present any other complaints. Uncomplicated atheroma is characterized by:
- painlessness;
- mobility;
- elasticity upon palpation.
The skin over the surface of the tumor is smooth and does not fold. The clinical picture may change when the contents of the atheroma become inflamed against the background of the addition of bacterial flora. In this case, patients may note:
- pain when pressed;
- redness and increase in size of the tumor itself;
- local increase in body temperature.
If the above symptoms occur, you should immediately seek help.
This situation threatens the penetration of infection into nearby tissues and blood with the spread of microorganisms to distant areas of the body and can cause a deterioration in the general condition of the child. Atheromas occur in areas of the skin that are rich in sebaceous glands. Therefore, they especially often have the following localization:
- scalp;
- face and neck area;
- shoulder girdle, armpit area;
- back.
Neoplasms occur less frequently in the groin area and scrotum (in boys). In these areas they have the appearance of a skin growth and require differential diagnosis with other skin tumors.
Skin syndrome in rheumatic diseases in children
Rheumatic diseases (RD) occupy one of the prominent places in the structure of childhood morbidity. According to consolidated reporting data from the Ministry of Health of the Russian Federation, the prevalence of rheumatic diseases is 5.7 per 100,000 children.
Rheumatic diseases of childhood are presented in the domestic working classification of the Republic of Belarus (1988-1998). These are rheumatic fever (rheumatism), diffuse connective tissue diseases, juvenile arthritis, systemic vasculitis, and other diseases of the joints, bones and soft tissues.
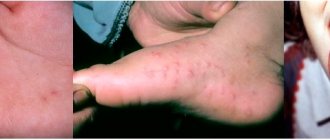
Among the clinical manifestations of a number of RBs, skin changes occupy an important place, the correct assessment and interpretation of which plays an important role in the differential diagnostic search and contributes to reliable and timely recognition of the disease.
This article highlights the features of skin syndrome in some rheumatic diseases of childhood observed by the authors.
Rheumatic fever
Rheumatic fever (rheumatism) is considered as a systemic disease of connective tissue with a predominant localization of the process in the cardiovascular system, developing in connection with acute infection with group A β-hemolytic streptococcus in predisposed individuals, mainly in children and adolescents 7-15 years old.
Diagnostic criteria include polyarthritis, cardiac involvement, chorea, erythema annulare, and rheumatic nodules.
Among the skin manifestations, ring-shaped erythema (annular rash) is observed in 7-10% of children, is usually not accompanied by subjective complaints, does not rise above the skin level, disappears with pressure, is predominantly localized on the skin of the torso, less often on the arms and legs. Ring-shaped erythema, as a rule, is noted at the onset of the disease; when activity subsides, it disappears, but it can also persist for a number of months.
Rheumatic nodules have been very rare in recent years, mainly in children with recurrent rheumatism. These are round, dense, painless formations varying in size from a few millimeters to 1–2 cm. The predominant localization is at the sites of tendon attachment, over bone surfaces and protrusions, in the area of the knee, elbow, metacarpophalangeal joints, in the occipital region and the area of the Achilles tendons. The number of nodules varies from one to several. They persist from 7-10 days to two weeks and less often - up to one month.
Neither erythema annulare nor rheumatoid nodules require special local treatment.
Juvenile rheumatoid arthritis (JRA)
From a modern point of view, JRA is considered as an independent nosological form of unknown etiology, characterized by complex autoimmune processes of pathogenesis, the presence of a large cascade of inflammatory and immunological processes developing on a genetically altered background and accompanied by systemic disorganization of connective tissue with the predominant involvement of joints in the pathological process and the progressive course of the disease.
The most serious variant in terms of the nature of clinical manifestations, course and prognosis is the systemic variant of JRA, which is divided into two forms: Still's disease and Wissler-Fanconi subsepsis.
Still's disease
It occurs, as a rule, in young children, usually begins acutely, is accompanied by hectic fever, a pronounced reaction from the reticuloendothelial system (lymphadenopathy, hepatolienal syndrome), involvement of internal organs in the pathological process (polyserositis), joint damage, and significant changes in laboratory parameters.
A classic sign of the systemic variant is the presence of skin changes in the form of a non-fixed erythematous rash, which is pink, maculopapular, less often pinpoint skin elements located on the chest, abdomen, arms, legs. They disappear with light pressure, are not accompanied by subjective manifestations and significantly intensify with fever and at the height of the activity of the pathological process. The rash often persists for a long time and may appear during exacerbation of the disease.
In 5-10% of children with the polyarticular form of JRA, the appearance of rheumatoid nodules is noted. Nodules of a dense-elastic consistency are usually mobile, not fused with the underlying tissues, the skin over them is sometimes erythematous. The nodules may disappear spontaneously or persist for a long time. Their appearance is considered an unfavorable prognostic sign.
Wissler-Fanconi subsepsis
It is an acute inflammatory condition, the characteristic features of which should be considered hectic fever, persistent rashes, arthralgia or unstable arthritis, hepato- and/or splenomegaly, lymphadenopathy, as well as high leukocytosis with a shift to the left, increased ESR and anemia in the blood. The disease picture resembles sepsis and Still's disease.
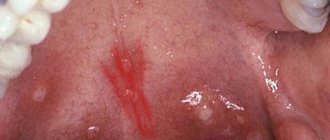
A characteristic manifestation of the disease is the presence of a rash, which is characterized by great diversity and polymorphism, often located on the torso and limbs. A typical sign of a rash is the Koebner phenomenon, i.e. the appearance or intensification of a rash in response to mechanical irritation of the skin. The rash is usually not accompanied by subjective complaints. A special variant of skin changes is characterized by a “linear nature”, and more often the stripes are located obliquely or horizontally, localized mainly on the torso and thighs, resembling stretch marks. A hemorrhagic rash is extremely rare.
A distinctive feature of the rash should be considered its stability. The rash worsens significantly as the temperature rises.
Systemic lupus erythematosus (SLE)
A multisystem autoimmune disease that develops on the basis of a genetically determined imperfection of immunoregulatory processes, which results in damage to many organs and systems. The main signs of SLE are skin changes, nonerosive arthritis, nephritis, encephalopathy, pleurisy or pericarditis, cytopenia (leukopenia and thrombocytopenia), and a positive test for ANA in the blood. There are more than 20 types of skin manifestations in SLE: from erythematous to severe bullous rashes. Most often (in 1/3-1/2 children), especially at the onset of the disease, erythema occurs above the zygomatic protrusions and in the area of the bridge of the nose, resembling a “butterfly”. It is characterized by symmetry and is usually not accompanied by any subjective sensations; worsens with excitement and solar insolation. Erythematous rashes are often located on open parts of the body in places not protected from the sun (face, upper chest), less often over large joints, mainly elbows and knees. Sometimes discoid lesions appear, leaving behind cicatricial atrophy. In the acute period, lupus cheilitis occurs (damage to the red border of the lips). Various vascular changes may also be observed: telangiectasia, palmar, plantar, digital capillaritis, hemorrhagic rashes, as manifestations of vasculitis (petechiae, purpura); livedo reticularis on the skin of the lower, less often the upper limbs and torso. Lupus enanthema or aphthous stomatitis occurs in 1/3 of children.
Scleroderma
In general, the disease is distinguished by clinical polymorphism. The most characteristic is the formation of scleroderma lesions of plaque or stripe shape, localized in various areas, most often on the limbs and torso. The lesions may be hypo/hyperpigmented, with a yellowish or reddish tint. Many children have a fairly pronounced thickening of the skin, which in some of them is combined with thickening of the subcutaneous soft tissues. Most patients have no subjective sensations, but itching and pain may occur. Over time, the lesions undergo a distinct transformation with the formation of residual changes in the form of atrophy and/or skin dyschromia.
In addition to plaque or strip-like skin lesions, rarer varieties are identified: “saber strike” type, Pasini-Pierini atrophoderma, white spot disease, bullous hemorrhagic, etc.
Children with systemic scleroderma have a more pronounced range of signs from the skin and subcutaneous soft tissues, and their relatively greater nonspecificity.
Dermatomyositis. Polymyositis
This is a severe progressive systemic disease of the muscles, skin and microvasculature with less distinct damage to internal organs, often complicated by calcification and purulent infection. The clinical picture includes fever, progressive muscle weakness, up to complete immobility, intense muscle pain, increasing muscular and general dystrophy.
Dermatitis is a pathognomonic sign for the disease, occurs in 3/4 of children with juvenile dermatomyositis, and most often appears within a few weeks of the onset of muscle symptoms. The most typical early skin changes can be considered erythematous spots with a violet tint, primarily in the periorbital (symptom of “glasses”) and perinasal areas, on the eyelids and ears, rashes in the area of the extensor surfaces of the small joints of the hands (Gottron’s papules), equivalents of which are also noted over other joints. Skin symptoms also include erythema with swelling of the periungual ridges, vasculitic spots, livedo reticularis, and ulcerative-necrotic changes. Alopecia and dystrophic changes in the nails may develop. The vascular component is represented by palmar capillaritis, livedo reticularis, and telangiectasia.
Systemic vasculitis
Systemic vasculitis (SV) is a group of diseases characterized by primary destructive and proliferative damage to the walls of blood vessels of various sizes, leading to secondary changes in organs and tissues. Existing classifications of SV take into account the caliber of affected vessels, the nature of inflammation, histological data, and immunological features of the process. Skin phenomena are included in various activity assessment schemes. These include: petechiae/ecchymoses, livedo reticularis, skin necrosis, ulcers, erythema nodosum, nodules along the vessels.
The most significant diseases from the group of systemic vasculitis in terms of the frequency of skin involvement are hemorrhagic vasculitis and polyarteritis nodosa.
Hemorrhagic vasculitis
The most common systemic vasculitis in children, characterized by damage to small vessels with changes primarily in the skin, intestines, and kidneys. Main manifestations: non-thrombocytopenic purpura, arthritis and arthralgia, abdominal pain, gastrointestinal bleeding and glomerulonephritis. In almost half of the cases, a recurrent nature of the process is noted. The prognosis is often favorable.
Almost all patients experience skin changes. Characterized by a symmetrical petechial rash and/or palpable purpura, localized mainly distally on the lower extremities, worsening after the child is in an upright position and observed for several days. These changes are so characteristic that they occupy one of the leading positions among other diagnostic criteria. Along with this, there are erythematous, papular and vesicular elements.
Polyarteritis nodosa
It is a necrotizing vasculitis of peripheral and central arteries of medium and small caliber. Juvenile polyarteritis nodosa is characterized by necrotization of the skin with underlying soft tissues and mucous membranes with the development of polymorphic clinical symptoms. Changes can affect any organ and develop against the background of fairly pronounced general symptoms of the disease (fever and cachexia). In addition, weight loss, skin changes, abdominal and musculoskeletal pain, and involvement of the central nervous system are noted.
Skin changes are observed in more than half of patients and are often one of the first symptoms of the disease. The most typical are painful subcutaneous nodules along the vessels, livedo (reticular or tree-like). Livedo, which occurs in most patients, can persist during periods of remission, becoming more pronounced during exacerbation. Every third patient develops thromboangiitis syndrome with the rapid formation of necrosis of the skin and mucous membranes, gangrene of the distal extremities. Papulo-petechial rashes, vesicles, and bullae may also be observed. The significance of skin changes in the diagnosis of the condition is emphasized by the presence of skin symptoms in the diagnostic criteria of the disease.
Lyme disease
It is a multisystem disease caused by the spirochete Borrelia burgdorferi, which is transmitted by ixodid ticks. Skin changes are represented primarily by tick-borne erythema migrans at the site of the tick bite. Erythema is a red spot growing along the periphery with a diameter of at least 5 cm, homogeneously colored or ring-shaped with clearing in the center. In a third of cases, erythema may be accompanied by itching and pain. Erythema may disappear spontaneously, but progression and chronicity of the process and the appearance of secondary skin erythema are possible. Quite rarely, the appearance of urticarial elements, erythema nodosum, a single benign lymphocytoma of the skin and, in adults, chronic atrophic acrodermatitis are also observed. Other clinical signs include influenza-like syndrome, enlarged regional lymph nodes, manifestations of the nervous system (damage to the facial and other cranial nerves and radiculopathy), heart (atrioventricular block), arthralgia, arthritis, and sometimes eye damage.
Skin changes occur in Kawasaki disease, mixed connective tissue disease, periodic disease and other rare diseases falling under the rheumatological rubric.
Treatment
Treatment of skin changes in most rheumatic diseases comes down to relieving the main symptoms of the disease. One of the leading places in the spectrum of antirheumatic drugs is occupied by glucocorticosteroids. The most intensive method of administering steroids is pulse therapy, in which the dose of the administered drug reaches 20–30 mg/kg per day. The course is three days, repeated administration is indicated if necessary. Doses prescribed orally vary depending on the nosological form and the degree of activity of the process from 1-2 mg/kg (calculated for prednisolone) to 0.5–0.7 mg/kg per day. A dose of 0.1–0.3 mg/kg per day can be considered maintenance. GCS are often prescribed in combination with NSAIDs in standard doses. Among the basic drugs that complement GCS, the drug of choice today (especially for JRA) is methotrexate (calculated dose 10 mg/m2 per week). Azathioprine (1.5 mg/kg per day), cyclosporine A (sandimmune) (3.5-5 mg/kg per day), cyclophosphamide, sulfasalazine, gold preparations, quinoline drugs, and their combinations are also used. A certain role in the treatment of rheumatic diseases is given to immunoglobulin therapy, which is carried out in courses of several cycles of intravenous administration at the rate of 0.4-0.5 g/kg per administration. Recently, there has been a search for new effective and safe drugs, such as necrosis factor inhibitors (Remicade, etanercept, etc.), mycophenolate mofetil, leflunomide, etc.
Local therapy is also used. Applications of DMSO, solcoseryl, indovazin, dollit cream, madecassol, heparin and other local remedies are prescribed. Physiotherapeutic procedures, including spa therapy, also play an important role. In many cases, the treatment complex includes antifibrotic drugs (penicillamine, as well as madecassol, colchicine, enzymes, etc.), glucocorticosteroids, and agents affecting the microcirculation system (pentoxifylline, nicoshpan, etc.). The need to use immunosuppressants (methotrexate, azathioprine, etc.), quinoline derivatives (plaquenil), and systemic enzyme therapy is discussed.
In dermatomyositis, sunscreens, anti-inflammatory and antipruritic drugs, and steroid ointments play a role in the treatment of skin changes. Quinoline derivatives are effective against dermatological manifestations of the disease. If skin changes are resistant, along with the use of GCS and plaquenil, dapsone, mycophenolate mofetil (allows you to gradually reduce the dose of GCS), tacrolimus (topical use for erythematous, edematous changes) can be added to the treatment complex.
Thus, skin changes, often an integral part of a complex picture of disorders throughout the body, occupy a significant place in the practice of pediatricians and pediatric rheumatologists. It is the skin syndrome, first detected at an appointment with a dermatologist or first contact doctor, that should alert you to the possible development of one of the rheumatological diseases.
D. L. Alekseev, Candidate of Medical Sciences N. N. Kuzmina, Doctor of Medical Sciences, Professor S. O. Salugina, Candidate of Medical Sciences Institute of Rheumatology RAMS, Moscow
Causes of atheroma in children
Atheromas in children occur due to a violation of the secretion of sebum by the corresponding glands.
When the excretory duct is blocked, the secretion of the gland has nowhere to go. It is secreted into the subcutaneous space, where a dense capsule is formed around it. Common causes of atheroma development in children are as follows:
- Using children's cosmetics (creams, ointments, moisturizing masks) in excessive quantities. Sometimes parents, in an effort to protect their child’s skin from harmful external factors, use cosmetic products uncontrollably. This leads to dysfunction of the sebaceous glands with blockage of their excretory ducts.
- Hormonal changes in the child's body. Infants and teenage children are traditionally at risk. It is during these periods that changes in the concentration of sex hormones occur. Against this background, acne appears, the function of the sebaceous glands is disrupted, and conditions are created for their blockage.
- Seborrhea. This is a dermatological disease that leads to dysfunction of the sebaceous glands in a certain area of the skin.
- Genetic predisposition or congenital structural features of the skin. Atheromas most often occur in children after 3 years of age. If neoplasms are detected in children immediately after birth, the doctor may assume the presence of problems with the sebaceous glands that developed in utero.
In addition, factors that increase the risk of developing atheromas are poor personal hygiene, metabolic disorders (obesity, diabetes) and frequent mechanical damage to the skin.
Diagnosis of atheroma in children
It is relatively easy to identify atheroma.
Even at the stage of the initial conversation with the patient or his parents, the surgeon assesses the general well-being of the child, collects anamnesis and analyzes complaints. When examining a neoplasm, the doctor pays attention to its size, location, pain, and the presence of redness. Before surgery, the surgeon prescribes a number of tests to comprehensively assess the child’s condition:
- general and biochemical blood test;
- general urine analysis;
- blood test for infections (HIV, syphilis, viral hepatitis B, C);
- ECG, fluorography.
The child is also examined by an anesthesiologist and pediatrician before the operation. A mandatory diagnostic method is histological examination of tumor tissue after its removal. At this stage, it is possible to determine whether it was an atheroma or a lipoma (a tumor similar in appearance).
Treatment of atheroma in children
The optimal method of treating atheroma in children is its surgical removal.
However, the age of the patient decides a lot here. Thus, most pediatric surgeons, in the absence of severe clinical symptoms, recommend a wait-and-see approach. Sometimes the swelling may resolve on its own. This is especially true for newborns and infants. In such cases, the development of the neoplasm is observed until the age of three, and if it persists, only then is it removed. Surgical intervention can be carried out traditionally using a scalpel or minimally invasively using a laser. In the first case, the surgeon excises the tumor with a capsule, which eliminates the risk of relapse. After this, cosmetic stitches are applied to the tissue to achieve the best aesthetic result.
Laser removal in children is used for small tumors. Using this technique, it is possible to avoid incisions and the formation of postoperative scars. In both cases, a comprehensive examination of the child is first carried out with the selection of the optimal treatment option.
In the postoperative period, the child may be prescribed the following groups of medications:
- painkillers;
- anti-inflammatory;
- antibacterial.
Drug therapy is aimed at eliminating discomfort and preventing infection of the postoperative wound.
Questions
- Which doctor treats atheroma in children?
A pediatric surgeon is involved in identifying and treating atheroma in children. - Is it possible to cure atheroma without surgery?
Sometimes in the early stages of the disease the surgeon chooses a wait-and-see approach. In 20-35% of cases, atheroma can resolve on its own. However, if the capsule is formed and the tumor is large, it will not be possible to do without surgical intervention. - How dangerous is atheroma in childhood?
Atheroma is a relatively safe tumor. It does not become malignant, rarely becomes complicated and is not accompanied by the development of permanent defects. However, this does not eliminate the need to consult a pediatric surgeon. Only a doctor can establish the correct diagnosis and select treatment. In addition, atheroma can sometimes become inflamed due to the addition of bacterial flora and cause a deterioration in the child’s well-being. - Is it possible to play sports after surgery?
After surgical removal of atheroma, it is recommended to refrain from active activities for 2-3 weeks. This will allow the tissues to fully heal and recover.
Features of hemangioma localization
As a rule, hemangioma is located on the child’s face: on the lip, on the cheek or on the forehead.
Since, according to statistics, this disease occurs more often in girls than in boys, the harm of a cosmetic defect can hardly be overestimated. However, there is localization of cutaneous hemangioma in children and on the scalp, on the limbs or on the torso. Moreover, it can be either single (1–2 spots in the field of view) or multiple, when a child has 3 or more hemangiomas, often combined with hemangiomas of parenchymal organs (liver, spleen, lungs and kidneys).