Lincomycin is a broad-spectrum antibiotic. And if you take into account the diversity of microflora in the oral cavity, it becomes clear why dentists often prefer this particular drug.
The action of lincomycin is based on the suppression of the vital activity of pathogenic as well as opportunistic microorganisms. Including staphylococci, viridans streptococcus and many other microbes resistant to other antibiotics. It is characteristic that microbial resistance directly to lincomycin develops over a fairly long time.
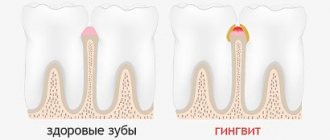
What is periodontitis
Periodontitis is an inflammation of the tissues surrounding the root of the tooth. Factors that contribute to the occurrence of periodontitis:
- Untreated caries, pulpitis;
- Chronic foci of infection in the oral cavity;
- Periodontal diseases;
- Chronic dental injuries.
Spicy
For acute periodontitis, a distinctive feature is the patient’s precise indication of the diseased tooth, as a feeling of “an overgrown tooth” appears, and only after a while unexpressed pain occurs. If the patient does not consult a doctor in a timely manner, general intoxication of the body, swelling of the gums and face may occur.
Chronic
The chronic process differs from the acute process in the absence of pronounced pain, and diagnosing such a tooth is sometimes only possible at an appointment with a dentist and during an X-ray examination.
Granulating
This type is determined only by x-ray examination, which determines the growth of granulation tissue in the area of the root apex.
Main contraindications for use
- severe dysfunction of the kidneys and liver,
- hypersensitivity to the drug,
- pregnancy and lactation.
This drug should not be used during pregnancy, as it passes through the placental barrier. In addition, this antibiotic passes into breast milk, so if treatment with lincomycin is necessary, breastfeeding should be stopped.
Lincomycin is a relatively “old” antibiotic, but despite this, it is very effective. That is why this drug is so valued in dental practice.
How to treat periodontitis
Stages
- On the first visit, it is necessary to take an x-ray to assess the stage of the disease and determine the form of periodontitis. Next comes the treatment of the tooth, providing access to the canals, actually working with the canals, and administering medications. Treatment of the canal in this disease is carried out repeatedly, at certain time intervals and under X-ray control. Permanent canal filling is carried out only if the doctor is completely confident that there are no pathological processes or complaints from the patient in the given tooth. Sometimes the terms last up to six months,
- During subsequent visits, permanent filling of the canals is performed.
- The final stage of periodontitis treatment is restoration of the anatomical shape of the tooth.
Each stage of periodontitis treatment is accompanied by diagnostic images! The number of visits depends on the anatomical structure of the tooth and the general condition of the body as a whole. And it is important to carry out an x-ray examination after 8-10 months to ensure the restoration of bone tissue.
Methods
- The therapeutic method consists of treating the canals using medicinal and mechanical methods. The main goal of this treatment is to preserve the tooth for many years. The success of such treatment largely depends on the patient’s timely visit to the doctor, the state of the immune system, and the availability of a qualified specialist.
- The surgical method is used when therapeutic treatment does not bring positive results. The most radical method is tooth extraction, but there are also a number of tooth-preserving procedures, which include resection of the apex of the tooth root, hismisection, cystotomy, and cystectomy.
Indications for use
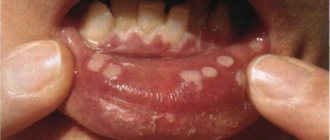
- gingivitis,
- periodontitis,
- periodontitis,
- osteomyelitis,
- periostitis,
- bone grafting of the jaw,
- dental implantation, etc.
In the treatment of inflammatory processes in the oral cavity, lincomycin plays an important, but not decisive, role. That is why it is successfully used in complex treatment. For example, when treating periodontitis, first of all, it is necessary to remove the source and result of the inflammatory process, and lincomycin, in turn, helps the body recover and prevent various kinds of complications.
Release forms
The drug is available in the form of tablets, injection solution, ointment, and antibacterial self-adhesive tape. The choice of dosage form depends on the patient’s condition, the nature of the lesion and the extent of the process. The dosage should only be determined by a doctor.
- tablets are in most cases prescribed for prophylactic purposes after various dental procedures. The patient can independently use them at home in the dosage prescribed by the doctor.
- The ointment is also intended for outpatient treatment and is effective mainly for superficial lesions of the oral mucosa. Before using it, the lesion must be washed, pus and dead tissue removed, and then a thin layer of the drug applied.
- Self-adhesive strips are very convenient for superficial gum lesions. They are glued directly to the affected area. Within 8 hours, the active substance is constantly released and has a therapeutic effect.
- injections are prescribed in the most severe cases. Depending on the severity of the condition, injections are given intramuscularly, intravenously or into the gums. The latter method allows you to quickly deliver the drug to the lesion.
Non-surgical adjuvant therapy for the treatment of periodontal diseases
Periodontal disease is an umbrella term used to describe an infectious inflammatory process that can affect one structural element or a complex of periodontal elements. The structures that support the tooth are alveolar bone, periodontal ligament and root cementum. Periodontal diseases are mainly provoked by the action of dental plaque or microbial biofilm, which is a heterogeneous structure of pathogenic microorganisms. More than 500 species of microorganisms are considered potential etiological agents that provoke damage to periodontal tissues. In addition to them, viruses and fungi also play an important role in the pathogenetic process. As the disease occurs and progresses, pathogenic microorganisms colonize the gum area surrounding the tooth, and as a result of their impact on the tissue, a periodontal pocket begins to form. Up to 109 species of bacteria can be found in deep periodontal pockets, but despite the potential of many pathogens that are associated with periodontal disease, only a small number are associated with active disease.
Socransky et al divided pathogens involved in disease progression into two main groups: the “red” and “orange” complexes. The red complex includes the following Gram-negative anaerobic bacteria: Porphyromonas gingivalis, Treponema denticola and Tanneralla forsythia, while the orange complex consists of Prevotella nigrescens, Peptostreptococcus micros, Campylobacter rectus, Centruroides gracilis, Campylobacter showae, Eubacterium nodatum and Streptococcus constellatus. In addition, Aggregatibacter actinomycetemcomitans and Eikenella corrodens are closely associated with periodontal diseases. As a result of numerous studies, it has been established that in order to achieve a successful treatment result, one aspect of therapy must be aimed specifically at neutralizing these bacteria, the activity of which is directly related to the course of the disease.
Antibiotics
Systemic antibiotic therapy should be considered as an acceptable treatment option for patients with periodontitis. This approach is relevant for patients who are resistant to conventional disease therapy or who have the following health problems: the presence of an abscess, a compromised or weakened immune state, uncontrolled diabetes mellitus, the presence of signs and symptoms of systemic lesions, fever and lymphadenopathy. The choice of the most appropriate systemic antibiotic should be based on the results of culturing microorganisms and testing their sensitivity to a particular drug. Thus, it is possible to find out, firstly, what microorganisms are present in the affected area, and, secondly, to select the most effective and active agent. But it should be remembered that systemic antibiotic therapy should not be the only method of treatment, but only represent a segment of an integrated approach to examination, diagnosis and development of adequate systemic therapy. Antibiotic therapy, like any other treatment method, has its advantages and disadvantages. Since taking these drugs is a fairly well-known method of treatment, patients, as a rule, understand the main key points of this treatment, and without any problems agree to the proposed algorithm for the course of medications. But at the same time, patients can often confuse the official main names of medications, forget the dose, time, or even the very fact of taking them, thereby disrupting the effect of their action. Systemic antibiotics may cause side effects and gastrointestinal disturbances in the form of diarrhea or abdominal cramps. Other possible negative effects of drugs are associated with allergic reactions and the emergence of bacterial resistance to antibiotics during prolonged and uncontrolled use. Bacterial resistance is a major concern in medicine because it creates a number of other scientific and clinical dilemmas regarding the therapeutic trade-off between the risk of treatment and the potential benefit of antibiotics.
Systemic antibiotics reach periodontal tissues by extravasation from the blood serum, after which they pass through the junctional epithelium and lining of the gingival pocket to enter the gingival sulcus area. The effective concentration of the antibiotic when it reaches the gingival sulcus during a course of treatment differs from that in any other tissue system or organ with signs of infection, which is associated with the specific structure of the periodontium. There are a number of well-tested antibiotic regimens for the treatment of periodontal diseases, which are usually used in combination with mechanical removal of supra- and subgingival deposits and bacterial plaque. This approach, combined with effective home oral hygiene, is aimed at reducing the bacterial load in the area of the gum tissue above and below the marginal border. Some physicians commonly prescribe antibiotic regimens for the treatment and management of periodontal disease based on amoxicillin (375 mg) and metronidazole (500 mg) taken 3 times a day for 7 days in combination with oral scaling and complete root planing for the first time. 48 hours. This approach helps to achieve a reduction in pocket depth and reduce bleeding, which was found when comparing treatment results in the study and control groups. An alternative treatment regimen is to take azithromycin (500 mg) for 3 days prior to scaling and root planing to reduce red complex bacteria and reduce gingival scores. In the absence of the ability to culture bacteria and determine their sensitivity to antibiotics, you can use the empirical principle of prescribing drugs for the treatment of periodontitis. Evidence-based treatment options include a combination of amoxicillin and metronidazole (250 mg - 500 mg each) taken 3 times a day for 8 days, or a combination of metronidazole and ciprofloxacin (500 mg) for 8 days, 2 times a day.
Topical antibiotic therapy is an alternative adjuvant treatment option that can also be used during the treatment of periodontal lesions. The essence of the procedure is to deliver the antibiotic directly to the periodontal pocket - that is, directly to the site of colonization of pathogenic bacteria, while the concentration of the antibiotic in the affected area increases markedly compared to systemic administration. Another advantage is the absence of potential gastrointestinal disorders and allergic reactions. The first antibiotic used for topical treatment was Actisite (periodontal tetracycline). It consisted of non-resorbable, tetracycline-impregnated fibers that were placed directly into the periodontal pocket and remained there for 10 days until the next visit to the dentist. Over time, drugs and methods of their delivery to the area of periodontal lesions have been improved. Thus, Atridox (Denmat) was developed, which is the first resorbable topical antibiotic consisting of a gel form of doxycycline. This drug is injected into the pocket using a syringe, and upon contact with saliva, it hardens, acquiring a waxy consistency. Thus, the antibiotic can be released from the solidified phase within 21 days. Arestin (Orapharma) is also a topical absorbable antibacterial that consists of minocycline granules in powder form. It is supplied in the form of ampoules charged into a syringe. The powder is injected directly into the periodontal pocket, the high level of its therapeutic effect continues for 14 days, and the drug itself remains in the pocket for 28 days. Studies have proven that the use of topical antibiotics together with the procedure of complete removal of tartar and root surface cleaning allows to achieve clinically effective results: a decrease in the depth of the pockets and partial restoration of the damaged biological attachment are observed.
Antimicrobial mouth rinses
Antimicrobial rinses are well-known and acceptable procedures that effectively complement the comprehensive treatment of gum tissue inflammation. Examples of their justified use are situations where the patient is unable to provide optimal oral care using conventional hygiene products at home, for example, in the postoperative period. To choose the right mouth rinse that will effectively cope with gum inflammation and at the same time prevent plaque, you need to find out whether it has a Certificate of Approval from the American Dental Association. If yes, then this product has gone through a series of clinical, biological and laboratory tests that have proven its anti-inflammatory and antibacterial effectiveness. However, it should be understood that this assessment is advisory, but not prescriptive regarding the drug. The only rinses available on the market with the appropriate rating of the Association are representatives with phenolic components, such as Listerine and other similar versions. Chlorhexidine gluconate (0.12%) is also considered the gold standard among antimicrobial rinses, which is available only by prescription in the United States and is known under the commercial names Peridex and PerioGuard (Colgate-Palmolive). Chlorhexidine is the most effective antimicrobial rinse, reducing bacteria and providing effective treatment for gingivitis. The drug is more effective against gram-positive bacteria and yeast, and less effective against gram-negative pathogens. It is usually prescribed postoperatively to reduce the bacterial load during the healing period. Chlorhexidine has a high substance content, which ensures its prolonged action. Some side effects associated with the use of chlorhexidine include potential staining of the teeth and dorsum of the tongue; change in taste perception; the risk of possible formation of supragingival stone, the formation of signs of mucositis and desquamation of the epithelium. Other antimicrobial rinses available to the general public, but less often recommended by specialists, are quaternary ammonium derivatives such as Cepacol (Reckitt Benckiser). Sanguinarine-based products, like Viadent, are no longer widely available on the market. Oxygenate-based products, such as hydrogen peroxide, are recommended to be used more often in paste form. They have anti-inflammatory properties, which reduce signs of bleeding. The latter is an important critical indicator for assessing periodontal inflammation. However, these representatives have only a small effect on the level of bacterial contamination, and recently opinions have increasingly been expressed about their possible carcinogenic potential. Triclosan is another antimicrobial agent available in the form of toothpastes and rinses. However, according to research, it also shows minimal effects on the microbial flora of the oral cavity, and the safety of its use is still in question.
Anti-inflammatory agents
We must remember that periodontal diseases are infectious in nature, and inflammatory phenomena are the body's immune response to microbial contamination. In inflamed tissues, the process of proliferation of pathogenic bacteria occurs faster, which leads to the progression of pathological and destructive effects of the inflammatory process, through the activation of cells of the body's immune system (macrophages and their precursors, monocytes, lymphocytes, and polymorphonuclear leukocytes, such as neutrophils). Components of the microbial structure, such as lipopolysaccharide, which is found in the cell walls of gram-negative anaerobic microorganisms, activate macrophages to produce and secrete proinflammatory cytokines such as interleukin-1 (IL-1) and tumor necrosis factor-alpha (TNF-alpha). Interleukin-1 stimulates bone resorption and also promotes the release of PGE2 by fibroblast cells, which are the main and most abundant types of connective tissue cells. Fibroblasts synthesize collagen, the main structural protein of connective tissue, which is also the main component of gum and bone fibers. These cells and inflammatory response cells (neutrophils and macrophages) synthesize matrix metalloproteinases (MMPs), which are enzymes or proteins involved in a number of biological reactions. For example, MMP-1 and MMP-8 are enzymes that are involved in the degradation of collagen, which significantly weakens the periodontal structure. Activation of the immune system is inherently a protective reaction of the body - a response to bacterial invasion, however, during the mechanism of implementation of the immune response, tissues of the host organism itself are destroyed. This phenomenon is associated with the release of cytokines, pro-inflammatory mediators and MMPs, since these agents act not only locally on periodontal tissue, but when entering the bloodstream they can also cause undesirable systemic effects.
MMPs are a group of proteolytic enzymes found in periodontal tissues, which contain collagenase and gelatinase. The function of these enzymes is to remodel the extracellular matrix. Since doxycycline was found by researchers to have anticollagenlytic properties, they proposed its use as a modulatory agent for the treatment of periodontitis. Subantimicrobial doses of doxycycline (20 mg twice daily) are effective in inhibiting collagenase activity while having no effect on antimicrobial resistance when used in combination with complete scaling and root planing. This approach provides the maximum effect for restoring biological tissue attachment and reducing the depth of periodontal pockets.
Oral medications
Nonsteroidal anti-inflammatory drugs (NSAIDs) have also been studied as inhibitors of the host response in the treatment of periodontal disease. Their mechanism of action is to prevent the production of prostaglandins. Prostaglandin E2 (PGE2) is directly associated with the processes of inflammation and bone resorption, which is confirmed by its verification in affected periodontal areas. In the course of studying various NSAIDs (flurbiprofen, ibuprofen, ketorolac, naproxen, aspirin), which were administered systemically or locally, it was found that when they were combined with the procedure for complete removal of plaque and root surface cleaning, it was possible to maintain the existing height of the alveolar ridge, preventing it resorption. Bisphosphonates are a class of drugs that inhibit alveolar bone resorption that have also been used as host-modulating agents in the treatment of periodontal disease. Studies have shown that bisphosphonates, when used in conjunction with full mouth cleaning, reduce periodontal pocket depths and levels of bleeding during probing, as well as improve restoration of biological attachment and maintain ridge height. However, despite the potential benefits of bisphosphonates, studies have shown that long-term use and high doses of the drugs initiate osteonecrosis of the jaw. Obviously, for reasoned conclusions, it is necessary to conduct further more detailed studies that will help determine the ratio of the potential benefits of drugs and the relative risk of complications in the treatment of periodontitis.
Host modulation therapy
Local application of host-modulating agents, such as enamel matrix proteins, bone morphogenetic proteins and platelet-derived growth factors, can be quite effective in the complex treatment of periodontitis. Enamel matrix proteins are available in the form of Emdogain (Straumann) and have been successfully used in the restoration of periodontal defects. These proteins play the role of healing modulators, stimulating the regeneration of all periodontal components of the supporting apparatus of the tooth. Bone morphogenetic proteins promote the modulation and differentiation of mesenchymal cells into bone progenitor cells. They act as a scaffold onto which new bone tissue can grow and are often used in guided bone regeneration during alveolar ridge augmentation. Finally, platelet-derived growth factors enhance the chemotaxis of neutrophils and monocytes, stimulate the proliferation of fibroblasts and, accordingly, the synthesis of the extracellular matrix, and also increase the level of differentiation of mesenchymal progenitor cells, fibroblasts and endothelial cells. It is platelet-derived growth factors that are most often used during surgical interventions on periodontal tissues in order to accelerate their regeneration.
conclusions
New knowledge regarding host-bacterial interactions and host immune responses that provoke periodontal tissue damage will be useful for the development of newer and more effective concepts for the treatment of periodontitis using systemic and local antibiotics, antimicrobial rinses and principles of host-modulating therapy. The results of further studies may shed light on auxiliary adjuvant therapy, which can be used to correct treatment algorithms in order to achieve the most successful effect of complex therapy for lesions of the supporting apparatus of the tooth.
Posted by Alison Glascoe, DDS, MS