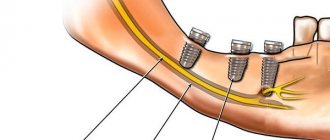
The facial nerve performs an important function - it provides movement in the facial muscles. It is thanks to him that we can express emotions without words and make grimaces - scary or funny. The facial nerve also controls the stapedius muscle, which protects the ear from loud sounds, ensures the perception of taste by the anterior two-thirds of the tongue, and increases the secretion of saliva. With neuritis, these functions are disrupted.
Our expert in this field:
Vasinkina Inna Yurievna
Neurologist
Call the doctor Reviews about the doctor
Some facts about facial neuritis:
- Another name for the pathology is Bell's palsy. It is associated with the name of the Scottish anatomist Charles Bell, who first described the disease in 1821.
- The disease has different prevalence in different regions and occurs more often in the cold season.
- In the United States, approximately 40,000 people are diagnosed with the disease each year. In the UK this figure is 25-35 people per 100,000 population. In general, Bell's palsy is considered a rare condition.
- You can get sick at any age, but most often neuritis of the facial nerve occurs in people 15-60 years old.
- Men and women get sick approximately equally often.
Suddenly experienced paralysis of one half of the face? Contact your doctor as soon as possible. This could be facial neuritis or a more serious condition such as a stroke.
Treatment of neuritis of the facial nerve
It is currently believed that the most effective treatment for facial neuritis is the use of glucocorticoids (drugs of adrenal hormones). They effectively suppress inflammation, which significantly speeds up the recovery of the affected nerve. The drug prednisolone is used in the form of tablets; the course of treatment usually lasts 10 days. In no case should you self-medicate: glucocorticoids are hormonal drugs, they have serious side effects.
Rehabilitation is of great importance - a set of measures that help restore impaired functions. Rehabilitation measures include:
- Thermal procedures are usually used after the 5-7th day from the onset of neuritis. A neurologist can prescribe mud, ozokerite, and paraffin applications.
- Ultrasound with hydrocortisone, which is also a drug of adrenal hormones.
- B vitamins – help improve nervous system function.
- Acupuncture.
- Massage and therapeutic exercises of facial muscles are prescribed after the symptoms of the disease subside.
We will call you back, leave your phone number
Message sent!
expect a call, we will contact you shortly
How long does it take to treat facial neuritis? What are the forecasts?
In most cases, the prognosis for facial neuritis is favorable - approximately 75% of patients make a full recovery. If treatment is carried out and the symptoms of the disease do not go away for more than 3 months, then the chances of full recovery are greatly reduced.
If, nine months after the onset of the disease, severe symptoms persist, the neurologist may recommend the following treatment methods:
- Mem therapy is a special set of exercises that helps strengthen facial muscles and improve movements in them.
- Plastic surgery. Improves the appearance of the face, but does not solve the nerve problem.
- Botox injections - in some cases, can help, in combination with therapeutic exercises.
Treatment should begin as soon as the first symptoms appear. Early initiation of therapy increases the chances of full recovery. Make an appointment with a neurologist at the Medical Center International Clinic Medica24 by phone.
We will call you back, leave your phone number
Message sent!
expect a call, we will contact you shortly
The main function of the facial nerve is to innervate the facial muscles. It provides facial expressions, movements of the lips, eyelids. It is also responsible for the following functions:
- Taste sensitivity of the anterior two-thirds of the tongue.
- Innervation of some salivary glands – increased secretion of saliva.
- In part, the facial nerve takes part in providing sensitivity to the oropharynx and skin.
- Innervation of the stapedius muscle in the middle ear (tympanic cavity). It limits the mobility of the auditory ossicles and thereby protects the ear from injury from loud sounds.
Accordingly, the symptoms of facial neuritis represent disorders of these functions. The most striking manifestation is a violation of movements in the facial muscles.
The facial nerve is a pair, that is, a person has two of them - on the right and on the left. Most often, neuritis occurs on one side. Much less often it is bilateral.
Symptoms of neuralgia
- Facial pain (prosopalgia). A characteristic sign of neuralgia. Sharp and sudden, reminiscent of an electric shock. Usually lasts from 5 to 15 seconds, is paroxysmal in nature and can occur at any time. During periods of remission, the number of attacks decreases. Most often, pain occurs in the area of the cheekbones and lower jaw (both right and left), and can be localized in almost all areas of the face.
- Impaired sensitivity. A severe form of neuralgia can lead to partial or complete loss of sensitivity of the skin.
- Nervous tic of the eyelid (nystagmus), spasms and twitching of facial muscles.
- Loss of coordination and motor skills are rarer manifestations of severe forms of the disease.
- Headaches, fever, chills and weakness are syndromes caused by viruses and infections.
What symptoms occur with facial neuritis?
The main manifestation of the disease is sudden paralysis of the muscles on one side of the face. This becomes especially noticeable when a person tries to frown, smile, or bare his teeth. The face becomes asymmetrical. In approximately two out of a hundred patients, paralysis of the facial muscles occurs on both sides at once.
This picture is reminiscent of another serious condition – stroke. You shouldn't self-diagnose. It is better to immediately call an ambulance. After all, with a stroke, literally minutes count – treatment must begin immediately.
Other possible symptoms of facial neuritis:
- It is difficult to close the eye on the affected side. This condition is called lagophthalmos (in medical jargon - “hare's eye”).
- Excessive salivation occurs.
- Due to the fact that the eye is constantly open, lacrimation and dryness occur.
- Impaired taste perception.
- Pain and discomfort in the ear area on the affected side.
- Increased sensitivity to sounds, loud ones are perceived painfully. In medical language this is called hyperacusis.
Each of these symptoms can be more pronounced or weaker; they are combined differently, depending on which part of the facial nerve the neuritis occurs on.
Proven fact: the success of treatment for facial neuritis directly depends on how early it is started. Therefore, you need to consult a doctor as soon as the first symptoms appear. In neurology at the international clinic Medica24, medical care is available without holidays or weekends.
Trigeminal and facial neuralgia
Neuralgia is a disease in which damage or compression of the trigeminal nerve and/or its branches occurs. This causes a sharp piercing pain that occurs suddenly and brings physical and psychological discomfort to the patient. Despite the fact that the term “neuralgia” can be literally translated as “nerve pain,” the matter is not limited to pain. Trigeminal and facial neuralgia are radically different in symptoms. The facial nerve contains mostly motor fibers, so neuralgia leads to dysfunction of the facial muscles (the degree depends on the severity of the disease), and can also cause lacrimation, dry eyes and partial loss of taste. Pain in facial neuralgia is usually concentrated in the area of the parotid gland (the patient complains that the pain radiates to the ear), but there may be no pain at all. It is because of the lack of pain that some experts use the term “neuropathy” when talking about damage to the facial nerve. With the trigeminal nerve it’s exactly the opposite, since it contains many sensory fibers.
What complications can occur with neuritis of the facial nerve?
In most cases, complete recovery occurs, all nerve functions are fully restored. With severe damage, some complications may occur:
- Involuntary contractions of some muscles due to improper restoration of nerve fibers. For example, when a person tries to smile, his eye closes.
- Loss of sense of taste.
- Ulceration of the cornea. It occurs when the eye is constantly open for a long time and the cornea dries out. In order to prevent this, the doctor prescribes special eye drops - “artificial tears”. Ulceration of the cornea can lead to infection and visual impairment.
- "Crocodile Tears" . There is increased lacrimation, the eye on the affected side constantly “cries”. Usually this symptom goes away after recovery, but sometimes it persists for a very long time.
An experienced neurologist will correctly assess the symptoms of facial neuritis and prescribe effective treatment and rehabilitation. Visit a neurologist. At the Medica24 international clinic, administrators accept calls any day 24 hours a day, please contact us.
We will call you back, leave your phone number
Message sent!
expect a call, we will contact you shortly
The cause of the development of neuritis of the facial nerve is its inflammation. The inflammatory process leads to damage to nerve fibers and disruption of their functions. Why is this happening? Scientists cannot fully answer this question. But there are some considerations.
Causes
Unlike neuritis, neuralgia is not an inflammatory disease. Fever, fever, swelling and other symptoms of the inflammatory process are not associated with this disease. However, if the trigeminal nerve is damaged due to neuritis, pain sensations that fit the description of neuralgia may well occur. To avoid confusion and differentiate the two pathologies, it is necessary to consider their etiology.
The cause of neuritis (like any other inflammatory disease) is viruses and infections that cause gradual destruction of the membrane and nerve trunk, and classical neuralgia in the vast majority of cases occurs due to mechanical effects on the nerve. Today, experts identify dozens of factors that provoke the development of the disease.
Main causes of neuralgia
- Head injuries leading to changes in the cranial structure and displacement of bones.
- Benign and malignant tumors that, as they grow, compress the trigeminal nerve.
- Various bite pathologies and other dental anomalies.
- Pathologies of the structure and diseases of blood vessels located in close proximity to the nerve (atherosclerosis, aneurysm, vasodilatation, etc.).
- Sinusitis and otitis in chronic form.
- Trigeminal neuralgia after tooth extraction. Occurs during a traumatic or incorrectly performed extraction procedure.
- Damage as a result of infection resulting from a number of diseases: periodontitis, periodontitis, stomatitis, herpes, syphilis.
Trigeminal neuralgia from hypothermia occurs rarely. However, this factor contributes to the development of the disease and complicates treatment. The same can be said about decreased immunity, metabolic disorders, neurosis, diabetes and other complicating factors.
The main cause of facial neuritis is infection
Experts believe that the main cause of the disease is a viral infection. Neuritis can be caused by the following infectious agents:
- Herpes viruses are pathogens that cause simple and genital herpes.
- The varicella zoster virus also belongs to the herpesvirus family.
- Another representative of this family is the Epstein-Barr virus , which causes infectious mononucleosis.
- Cytomegalovirus is a member of the herpes viruses that causes cytomegalovirus infection.
Facial neuritis is also associated with borreliosis (Lyme disease), a bacterial infection. Similar symptoms occur with the pontine form of polio.
Classification of the disease
Due to the occurrence
- Primary (idiopathic) trigeminal neuralgia. A classic type of neuralgia, so to speak. Occurs due to compression of the trigeminal nerve.
- Secondary trigeminal neuralgia is a consequence of other diseases and viruses.
By coverage
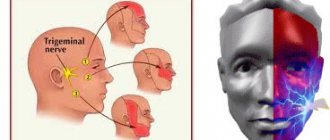
- Unilateral (one branch of the trigeminal nerve is affected).
- Bilateral (more than one branch is affected).
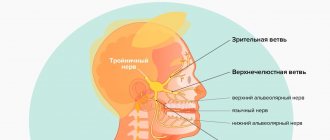
Neuralgia can affect the 1st, 2nd, 3rd branches of the trigeminal nerve. The first branch is responsible for the orbital zone, the second for the median zone (including the nose and upper lip), and the third for the lower jaw. Most often, damage to the third branch is diagnosed, so the pain affects the area of the lower jaw, and an attack often occurs during hygiene, eating or shaving.
Other conditions that may lead to illness
There are some known factors that are thought to contribute to the onset of the disease:
- Hypothermia. Manifestations of the disease can occur after being “blown out” while driving in a car with an open window, or sleeping near an open window.
- Head injuries.
- Atherosclerosis, arterial hypertension - these diseases lead to impaired blood circulation and nerve nutrition.
- Impaired blood flow in the vertebral artery - the cause may be osteochondrosis, intervertebral hernia in the cervical spine.
- Unsuccessful anesthesia in dentistry when the tip of the needle hits a nerve.
Sometimes you can hear that vaccination can be the cause of facial neuritis. However, studies have proven that there is no connection between vaccinations and this disease.
International Clinic Medica24 is a modern clinic where medical care is available around the clock.
How does treatment depend on the cause?
Until 2007, experts debated which types of treatment for facial neuritis were most effective. Some insisted on the use of antiviral drugs, since the disease is most often caused by a viral infection, others preferred glucocorticosteroids (hormonal drugs that have a powerful anti-inflammatory effect), while others argued that their combination works better.
After clinical studies, it was decided that glucocorticoids are most effective.
Only a neurologist can correctly determine the cause of the disease and prescribe effective treatment. Visit a doctor as soon as the first symptoms begin to bother you. Make an appointment with a neurologist at the Medica24 international clinic by phone.
We will call you back, leave your phone number
Message sent!
expect a call, we will contact you shortly
The main manifestation of facial neuritis is paralysis of the facial muscles. It usually occurs on one side, but in 2 out of 100 patients it occurs on both sides. This symptom is not unique to facial neuritis. It can also occur with other diseases: stroke, certain infections, Lyme disease, cancer.
An experienced neurologist will be able to understand the causes of facial paralysis and prescribe timely treatment that will help.
Types of trigeminal neuralgia
There is an additional classification that can also be used in making a diagnosis.
Acute
Acute trigeminal neuralgia, accompanied by frequent and severe attacks.
Chronic
Chronic trigeminal neuralgia is a consequence of an untreated disease. The patient has been observed for a long time: remissions alternate with exacerbations.
Atypical
Atypical trigeminal neuralgia occurs against a background of stress and nervous exhaustion (psychosomatics).
Postherpetic
Postherpetic trigeminal neuralgia occurs after a history of herpes and its symptoms differ from the classic type. The pain is usually burning and may not go away for two to three hours.
Diagnosis of facial neuritis in the clinic: what happens in the neurologist’s office?
During the conversation, the doctor may ask you the following questions:
- When did you notice that you had facial paralysis? How did this happen - abruptly, unexpectedly, or gradually?
- Have you recently had any infectious diseases?
- Have you had similar problems before? Has anyone in your immediate family suffered from Bell's palsy?
- What other complaints do you have?
- Are you bothered by pain in the face or ear?
- Do you taste food well?
Next, the doctor will conduct a general neurological examination, since manifestations of facial neuritis may be caused by another, more serious disease. You will be asked to raise and frown your eyebrows, smile, bare your teeth, stick out your tongue - these tests will help determine the dysfunction of the facial muscles. If after the examination the doctor finds it difficult to establish an accurate diagnosis, you will be prescribed additional diagnostic methods.
The international clinic Medica24 employs experienced neurologists and uses uniform standards developed by experts. You will be carefully examined, all necessary procedures will be prescribed in your case, and an accurate diagnosis will be established.
Diagnosis of the disease
Modern medicine has in its arsenal many diagnostic techniques that make it possible to determine the type of neuralgia and the cause of its occurrence:
- visual examination and questioning of the patient;
- X-ray of the jaw;
- MRI of the brain and blood vessels;
- laboratory analysis of urine and blood;
- electromyography.
Diagnosis is carried out by a neurologist, but additional examinations by other specialists are often required: dentist, ophthalmologist, otolaryngologist. Particular attention is paid to differential diagnosis, since neuralgia may resemble other diseases in its symptoms, in particular glaucoma, otitis media, ethmoiditis, Slader syndrome, etc.
Additional methods for diagnosing facial neuritis at the international clinic Medica24
Electromyography is a study during which, using special electrodes, the nature and quality of signal transmission along the nerve and muscle response are determined. This helps identify facial nerve damage and the level at which it occurred.
Imaging tests – Your doctor may order a CT scan or magnetic resonance imaging scan. These studies help in diagnosing some conditions that lead to symptoms of facial neuritis, for example, skull fractures, cancer.
If the neurologist believes that your complaints could be caused by diabetes or an infectious disease, you will be prescribed appropriate laboratory diagnostic methods.
Private medicine often suffers from the fact that doctors try to prescribe as many diagnostic procedures as possible to patients, “just in case.” At the Medica24 international clinic, you will be prescribed only those tests that are necessary in your situation. We even have specialists - coordinating doctors who make sure that each patient receives full medical care, but does not overpay for anything unnecessary. Our main value is your health.
The Medica24 international clinic is a place where experienced professionals work and use the most modern diagnostic methods, allowing you to quickly establish a reliable diagnosis. We work around the clock, call at any time.
The material was prepared by Natalya Yurievna, a neurologist at the international clinic Medica24, Candidate of Medical Sciences Lasch.
Presentation “Neuropathy of the facial nerve” presentation on the topic
Slide 1
Neuralgia. Facial nerve neuropathy. Prepared by: Derbilova A.V.
Slide 2
Neuropathy is a disorder in the transmission of nerve impulses along a nerve (death, insufficient blood supply, or compression of the nerve). Neuritis is inflammation of a nerve that can lead to neuropathy.
Slide 3
The facial nerve consists of three types of nerve fibers: those that travel from the brain to the facial muscles and ensure their contraction, sensory fibers that carry taste sensations from the anterior two-thirds of the tongue, and nerve fibers that control the salivary glands. Each type of fiber has its own center (nucleus) in the brain stem. On its way from the brain, the facial nerve passes through the temporal bone, in which there is a special canal for it.
Slide 4
Frequent causes of damage to the facial nerve inside the cranial cavity: Vascular problems are insufficient blood supply to the centers or their irritation by an overly tortuous artery, spasm of the arteries that supply blood to the trunk of the facial nerve; Consequences of head injury (damage to the temporal bone is especially dangerous); Anomaly of the temporal bone (excessively narrow canal of the facial nerve, leading to compression). Congenital neuropathy of the facial nerve occurs as a result of birth trauma or Moebius syndrome (congenital damage to the facial nerve in combination with damage to the abducens nerve and horizontal gaze paresis), in the latter case the lesion can be bilateral. Compression of the facial nerve root by a tumor; Lyme disease can cause facial neuropathy, often bilateral, in endemic areas following tick bites and chronic migratory erythema. HIV infection, even without manifestations of AIDS, causes one or bilateral damage to the facial nerve. Viral infection (herpes zoster). Damage to the facial nerve and geniculate ganglion with a rash of blisters on the auricle or in the external auditory canal (Hunt syndrome). In case of inflammation and swelling of the facial nerve, it swells and compresses itself in its narrow bony canal, and then dies from compression. This is precisely what is a common cause of facial paralysis.
Slide 5
Common causes of damage to the facial nerve after exiting the cranial cavity: Facial trauma; Inflammatory process, swelling of the salivary gland; local cooling, often in combination with influenza infection (Bell's palsy); Inflammatory processes in the middle ear play an important role in the development of neuritis; Metabolic or infectious damage to nerves (polyneuropathy); Sometimes after tooth extraction under mandibular anesthesia (pain relief in dentistry during interventions on the teeth of the lower jaw); Diabetes mellitus (insufficient supply of glucose and blood to the nerve).
Slide 6
Symptoms of neuritis, neuropathy of the facial nerve. Neuritis of the facial nerve is clinically manifested by facial asymmetry as a result of paresis or paralysis of the muscles of the corresponding half of the face. On the side of the nerve lesion, the folds of the skin of the forehead are smoothed or absent, the palpebral fissure is widened, the nasolabial fold is smoothed and lowered, the lower lip hangs down. When showing teeth or laughing, the mouth is pulled to the healthy side. When opening the mouth, the angle on the process side is sharper than on the healthy side. When the eyebrows are raised upward, horizontal folds of the skin of the forehead are not formed, since the eyebrow of the paralyzed side does not rise. When closing the eyes, the eyelids do not close completely and the palpebral fissure on the side of the nerve lesion gapes. The patient cannot stretch out his lips, whistle, or kiss. While eating, food gets stuck between the paralyzed cheek and teeth. Superciliary, corneal and conjunctival reflexes are reduced or absent. Depending on the level of nerve damage, the described picture is accompanied by signs of taste disturbance in the area of the anterior two-thirds of the tongue. A herpetic rash in the external auditory canal, increased tear production, and dry eyes are observed.
Slide 7
As a result of neuritis of the facial nerve, a disturbance in the conduction of nerve impulses from the brain to the facial muscles occurs, which is manifested by paresis or paralysis of these muscles.
Slide 8
Treatment of neuritis of the facial nerve Treatment is selected individually in each specific case. It includes a set of procedures: acupuncture, stimulation of the facial nerve and facial muscles (physical therapy and articulation exercises) UHF at the exit point of the facial nerve, vitamins “B”, “C” and “E” antiviral drugs, homeopathic remedies, etc.
Slide 9
In mild cases, facial neuritis may reverse within two to three weeks or even faster. In severe forms of paralysis, paralysis can be complicated by contracture of the affected muscles, manifested by a persistent increase in the tone of the facial muscles. Contractures of the facial muscles usually manifest themselves as a narrowing of the palpebral fissure, pulling upward the corner of the mouth on the affected side. In this case, unpleasant sensations and painful muscle spasms occur on the side of the paresis; it is important that any physical and emotional stress contributes to an even greater narrowing of the palpebral fissure and pulling up the corner of the mouth. In addition, lacrimation increases during chewing (a symptom of “crocodile tears”). At the same time, tics appear in the affected muscles. The result of treatment depends on how quickly the patient sought medical help, as well as on how carefully all recommendations for treatment and rehabilitation were followed.